How to Include Sibling Voices in Perinatal Loss Memorials
The Problem: The Forgotten Mourner in a Bereaved Household
Siblings of lost babies are named in the research literature as the "forgotten mourners." A study on sibling grief in perinatal loss describes how the attention and resources that flow to bereaved parents almost never reach their surviving children, even when those children are clearly grieving. A data point from Intermountain Health's membership in the National Trauma and Grief Network puts it sharply: one in fifteen children will experience the death of a parent or sibling by age 18. The volume is real. The infrastructure is not.
The AAP clinical report on supporting the grieving child describes trauma-informed support practices for bereaved siblings and emphasizes that children process loss through representation — drawings, songs, play — more than through verbal testimony. A PubMed systematic review of bereavement interventions for children after sibling death found that child-specific interventions are underresearched and underresourced, and that most published protocols target parents with siblings mentioned as collateral. The NCBI Bookshelf chapter on bereavement experiences after the death of a child describes sibling loss as one of the most difficult experiences a child can have, often compounded by parents whose own grief leaves them unable to attend to their surviving children.
And a SAGE study on parental behavior toward surviving siblings concludes that supportive parental behavior is the single strongest predictor of healthy sibling grief — but parents who are themselves drowning cannot be the only channel. Memorials have to make room for sibling voices directly.
Solution Framework: A Sibling Lane in the Tapestry
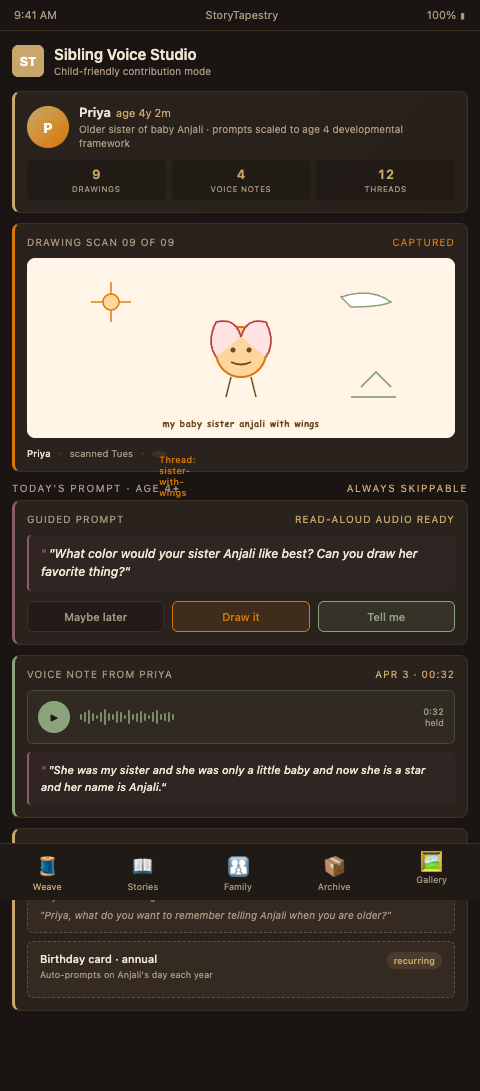
The tapestry metaphor extends to sibling inclusion cleanly: the sibling gets their own channel, their own materials, and their own pace. They are not editors of the parents' weave — they are weavers in their own right. StoryTapestry designs this as a dedicated sibling lane with age-appropriate capture tools, parent-supervised visibility, and long-term accessibility as the sibling grows.
Capture first. A three-year-old sibling cannot fill out a web form. A nine-year-old might write a paragraph but not a letter. A fifteen-year-old often has more to say than any adult in the household. StoryTapestry provides three capture modes. Drawing: a tablet-compatible drawing canvas that saves with a timestamp and an optional audio note ("tell me about this picture"). Audio: a one-button recording mode that captures what the child wants to say, with no transcription shown back so the child is not correcting themselves. Text: a simple text field with no word count, no auto-correct that flags misspellings as errors.
Parent supervision is built in but gentle. Contributions from any child under 13 route to a parent review queue before joining the visible tapestry. The review does not ask parents to edit — it asks them to confirm that the child understood the contribution would be visible to family, that the content is emotionally safe for the parent to re-encounter, and that the attribution is correct. Siblings 13-17 can publish directly with an after-the-fact parent notification. Over 18 operate with their own consent, per bereaved parent communities standards.
Developmental sequencing matters. A four-year-old's contribution to a baby's memorial at the time of loss, and that same person's contribution at fourteen, do not share anything except attribution. Both should persist. The tapestry preserves contributions as time-stamped threads so a sibling can look back at seven what they drew at three, and add to the memorial at twelve, seventeen, and thirty. This is the continuing-bonds framework in action: the memorial grows alongside the surviving child.
Shared rituals anchor sibling inclusion beyond one-off contributions. The hospital bereavement team can invite siblings into hospital-based rituals — placing a handprint next to the baby's footprint, selecting a blanket, choosing the name of the bear that accompanies the memory box. These shared physical rituals become photograph threads in the tapestry, giving the sibling a documented presence at the loss rather than an exclusion from it. Blended memorial customs programs developed for multi-faith households extend the same pattern to households where grandparents and extended family practice different rituals around the lost baby.
Handling memorial content disagreements becomes especially important when parents hold different views on sibling inclusion. The dual-channel approach — sibling content has its own lane, sibling decisions cannot be overridden by a single parent alone — protects the sibling's participation from becoming a second-order casualty of parent conflict.
Two design choices distinguish the sibling lane from a generic contribution channel. First, the prompts are explicitly child-directed rather than adult-directed. An adult prompt reads "share a favorite memory"; a sibling prompt for a five-year-old reads "what color was your sister's blanket?" or "what song did you want to sing for her?" The difference matters because children respond to concrete, sensory questions far more than to abstract memory prompts. Bereavement coordinators who sit with young siblings during capture describe the moment a child moves from frozen silence to animated answering when the question shifts from open-ended to specific. The prompt library is organized by age band and by loss context (stillbirth, NICU death, miscarriage with older siblings) so that coordinators can select the right question without improvising under emotional load.
Second, the sibling lane preserves child-generated content with its original imperfections. An adult writing a memorial will edit, revise, and spell-check; a child producing a drawing or voice note will not. The platform does not auto-correct, re-record, or clean up sibling contributions. A six-year-old's voice saying "I miss the baby that almost was my sister" is preserved with every hesitation and mispronunciation. A nine-year-old's handwritten note that spells her sister's name three different ways across three lines is preserved as scanned, not transcribed. The imperfection is the evidence of the child, and parents tell coordinators months later that the imperfect version is what they return to most.
Advanced Tactics for Age-Responsive Sibling Inclusion
Three tactics distinguish programs that include siblings well from programs that token-include them.
First, train intake staff on child-directed consent language. A bereavement coordinator asking a four-year-old "do you want to help make your sister's memorial?" gets different (and better) answers than a parent asking on the child's behalf. The AAP clinical report stresses that children respond to direct, age-adjusted invitations and often decline when questioned indirectly. StoryTapestry provides a coordinator-facing script library organized by age band (3-6, 7-10, 11-14, 15-18) so staff do not improvise under emotional load.
Second, build contribution rituals families can repeat. The annual anniversary and the sibling's own birthday are reliable prompts for a new thread. Programs that send a gentle notification to the parent suggesting "would Maya want to add something this year?" produce more consistent sibling participation than programs that rely on spontaneous parent-initiated contributions. Keep the notification opt-out, because some years the answer is no, and "no" is a valid contribution.
Third, prepare for sibling questions that shift across development. A child who at five asks "where is the baby?" will at eleven ask "what happened?" and at sixteen may ask "why did this happen to our family?" The tapestry stores the medical and narrative context in a way that is accessible at the depth the sibling is ready for, with parent-supervised reveals available when the sibling requests them. This aligns with the AAP clinical-report recommendation that information be made available across development, not delivered once.
Fourth, offer separate bereavement resources for the sibling that do not require parent participation. School counselors, pediatricians, and youth bereavement programs can be listed inside the sibling lane as optional resources the sibling can reach through with parent awareness but not parent gatekeeping. The SAGE paper on parental behavior and sibling grief supports this: siblings benefit from adults-beyond-parents in their grief landscape.
Fifth, partner with child-life specialists at every step. Hospital child-life specialists are trained in developmental trauma response and are often the most appropriate staff to lead sibling capture sessions. Many hospitals under-utilize their child-life team for bereavement work because the team is primarily assigned to pediatric medical units. A bereavement program that formally partners with child-life, allocates a fraction of a child-life specialist's time to perinatal bereavement, and funds that allocation through the bereavement program budget typically sees sibling participation rates double within six months. The specialist knows how to sit on the floor with a four-year-old and produce a drawing that the four-year-old understands will become part of a permanent memorial. Coordinators who try to substitute for this expertise without training produce sibling interactions that are well-intentioned but developmentally off.
Sixth, design the visibility toggle for the sibling's own privacy. A sibling who makes a contribution at age six may, at age fourteen, want some of their younger content made private from extended family viewing. StoryTapestry gives siblings who reach age thirteen their own account access with the right to retire any of their earlier contributions to a private vault — not to delete them, because the parent may still want to access them, but to remove them from public family viewing. This respects the developmental shift where young children contribute with full enthusiasm and teenagers often want more control over their earlier selves. The architecture does not force an adolescent to either accept their six-year-old drawing being publicly visible or to destroy it; it offers the third option of keeping it while moving it out of view.
Seventh, prepare for the sibling who does not want to contribute. Forced sibling inclusion is worse than no inclusion. Some four-year-olds and some fourteen-year-olds will decline to contribute, and the decline is itself information about how the sibling is processing the loss. Coordinators should not push, should not persuade, and should not ask again at every anniversary. The platform supports "the sibling declined" as a documented status with an option to revisit annually or never, at the sibling's choice. A sibling whose decline was respected at age five is significantly more likely to contribute at age twelve than a sibling who was pressured at every opportunity. Patience is infrastructure.
CTA: For Hospital Bereavement Programs Extending to Surviving Children
A perinatal loss is not a one-person loss, and your memorial program probably already knows this — but the siblings in your patients' families are still sitting on the couch at the funeral home with nothing to contribute. StoryTapestry gives your bereavement team a sibling-specific capture workflow, parent-supervised visibility for young children, and long-term threading that grows with the child.
Bring a social worker, a child-life specialist, and a bereavement coordinator to a 45-minute session. We'll walk through the four age bands, demonstrate the age-specific prompt library, and map your current intake gaps to the sibling-lane workflow. If possible, bring a de-identified recent case where a sibling was present in the family but absent from the memorial — these are the cases that most clearly illustrate what the sibling-lane workflow would have added.
Programs adopting the sibling lane typically pilot with a cohort of ten families who have surviving children under eighteen. The pilot runs six months and produces three artifacts: an age-banded prompt library tailored to your patient population, a child-life specialist allocation agreement with your pediatric team, and a set of age-appropriate consent forms reviewed by your compliance office. Coordinators finishing the pilot report that sibling inclusion becomes a regular part of their practice rather than an exception, and that the siblings themselves — now six months past loss, contributing their second or third thread on the anniversary — become the most consistent visitors to the tapestries in the program.