Future of Ambient Story Capture in Long-Term Care Settings
The Fragment Decay Problem
Long-term care settings produce hundreds of story fragments per resident per month — fleeting, unsolicited, often repeated. A review of lifelogging and episodic memory rehabilitation confirms what memory-care staff know experientially: daily fragments matter, and reviewing them improves episodic memory in Alzheimer's disease. Most of these fragments are lost because no capture infrastructure exists.
The stakes are not theoretical. Research on lifelogging wearable camera acceptability in MCI shows that older adults with mild cognitive impairment become competent lifelogging camera users, suggesting the technology is feasible. The barrier is design sensitivity — solutions that feel like surveillance will fail regardless of technical capability. A qualitative study of older adults monitored at home documents that residents feel shame when constantly watched, which means ambient capture must be designed around dignity constraints, not around maximum data collection.
The current options are unsatisfying. Staff write incident notes. Families send photo texts. Speech therapists capture assessment-window recordings. These are siloed, non-searchable, and tied to documentation workflows rather than narrative preservation. Long-term care operators and funeral-home partners need a third option: ambient capture designed specifically for memorial-adjacent story work, with privacy and dignity as primary constraints.
The clinical staff time cost is the second missing piece. CNAs and activities staff already document shift notes, incident reports, MDS assessments, and care plans. Asking them to additionally "write down stories" creates documentation burden they cannot absorb. A memory-care aide managing 12 residents on a 2pm-10pm shift does not have 20 uninterrupted minutes to transcribe a resident's spontaneous story about the 1957 harvest. Ambient capture solves this by doing the preservation work automatically and routing only approved, narratively-shaped fragments back to staff for brief confirmation. The cost to staff time drops from 20 minutes per fragment to 45 seconds per approval.
Ambient Capture as Slow Weaving
StoryTapestry's ambient capture module sits at the intersection of consumer technology, care-sensor infrastructure, and narrative preservation. Rather than recording everything, it listens for story-shaped utterances — personal anecdote structure, autobiographical references, extended narration — and flags these moments for optional capture with explicit consent. The default state is off; the activation state is opt-in at the individual, family, and facility level.
The tapestry metaphor holds: ambient capture provides long threads, gathered slowly, that interview-based capture cannot produce. An interview asks a caregiver to recall what the resident said; ambient capture preserves the resident's actual voice saying it. A 2014 study of dementia residents managing chaos through life storytelling found that residents in nursing homes actively tell stories to make sense of their new environment — ambient capture preserves this telling rather than requiring staff to write it down later.
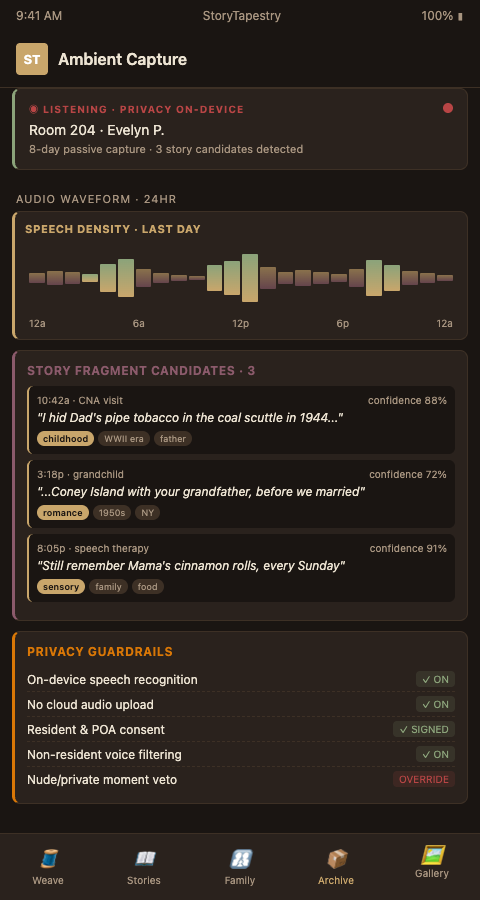
The technical stack uses voice activity detection plus narrative classifiers to distinguish story-telling from routine speech. A resident asking for water is not captured. A resident saying "my father never let me drive the tractor until I was 14" is flagged for review. The classifiers run on-device where possible, which reduces both bandwidth and privacy risk. Only fragments that pass narrative detection and reviewer approval are uploaded to the tapestry.
Privacy design is structural, not bolted-on. Ethics of sensor-based surveillance in dementia research documents strong preferences for radar and presence sensors over video surveillance. StoryTapestry follows this hierarchy: audio-only capture in common areas with posted notices, no capture in bathrooms or bedrooms without explicit per-resident consent, and no continuous recording — only flagged fragments saved. Ambient assisted living literature describes sleep mats and motion sensors as less intrusive monitoring options, and the same design sensibility applies here.
Multimodal sensing improves fragment quality. Research on multimodal wearable intelligence for dementia care documents how unobtrusive sensing across audio, location, and movement enriches context. StoryTapestry threads these modalities: a resident telling a tractor story in the garden produces audio + location fragments that the family sees as "told this on a Tuesday afternoon in the sunflower bed" — context that makes the fragment memorial-worthy.
PIR motion and contact sensors dominate ambient monitoring across care settings, which creates an installed base StoryTapestry can integrate with rather than displace. Facilities that already have presence sensing for fall prevention can add narrative capture as an additional layer without new hardware investments. This matters for adoption — long-term care budgets are tight, and additive integrations win over replacement projects.
The approach aligns with AI narrative assembly downstream: ambient fragments feed the threading engine alongside interview-based fragments, giving the AI a richer corpus. The multi-source case study reconstruction of Margaret's 40-year story would have been substantially richer if ambient capture had been running during her six years in memory care — dozens of unrecorded story-telling moments would have been preserved.
Facility deployment is staged. First, common-area audio capture in resident lounges, dining rooms, and garden spaces where conversations naturally happen. Second, opt-in personal capture for residents with consent and family sign-off, typically via a discreet wearable that activates during waking hours. Third, visitor-mediated capture during family visits, where family members use a tablet app that records structured interview moments alongside casual conversation. Each stage has its own consent workflow, retention rules, and reviewer pathway. Facilities that try to deploy all three simultaneously overwhelm their consent and review infrastructure; facilities that stage the deployment across 6-12 months absorb the operational complexity gradually.
Advanced Ambient Capture Decisions
Design consent as a ladder, not a checkbox. Residents may consent to ambient capture at admission while still cognitively intact, but capacity changes. StoryTapestry's consent ladder establishes proxy decision-making with the family at admission, documents the resident's capture preferences while capacity remains, and flags any fragment captured after capacity loss for proxy review before tapestry integration. This is both ethically necessary and legally defensible under most state long-term-care regulations.
Limit retention aggressively. Captured fragments that do not pass narrative classification within 72 hours are deleted. Captured fragments that the reviewer rejects are deleted immediately. Only approved, family-confirmed fragments persist in the tapestry. This retention discipline is what separates ambient story capture from surveillance — the default outcome of any captured audio is deletion.
Use staff as the first reviewer. Care staff already in the room with the resident are better positioned to decide whether an ambient fragment is story-worthy than a central reviewer. Build the workflow so the aide or nurse assigned to the resident receives flagged fragments at shift-end and approves, rejects, or escalates. This respects staff expertise and avoids the "remote voyeur" dynamic that kills ambient-capture adoption.
Segment fragments by confidence. Ambient capture is noisier than interview capture. Label fragments by classifier confidence — high (clear narrative structure, single speaker, minimal background), medium, or low — and use confidence to set reviewer prioritization. High-confidence fragments get immediate reviewer attention; low-confidence fragments are archived with a "not reviewed" flag that families can optionally revisit during tapestry construction.
Integrate with family portals for real-time access. Families whose loved one is in long-term memory care often cannot visit weekly. A portal where they can review approved fragments — and contribute family context that reframes what staff heard — turns ambient capture into an active family engagement tool, not only a memorial-prep tool. Families report that reviewing fragments between visits helps them feel connected during long cognitive decline.
Parallel modalities are emerging across memorial contexts. Wearable biometric capture adapts ambient-sensing logic to perinatal loss, where the capture window is compressed and the signals are different. The common principle — passive preservation of otherwise-lost moments with strict consent boundaries — transfers across memorial domains.
Plan for regulatory shifts. HIPAA and state long-term-care regulations will evolve as ambient capture becomes more common. Build the system with strong audit logging, per-fragment consent attribution, and deletion workflows that satisfy anticipated 2027-2028 compliance demands. Early movers who architect for future regulation avoid expensive retrofits.
Involve residents in designing their own capture boundaries. For residents still cognitively capable at admission, include a "capture preferences" interview as part of orientation: when do you want to be captured, what kinds of conversations, with which visitors, under what circumstances. Residents who co-author their own capture rules feel the system respects their agency rather than imposing surveillance. Preferences document into the resident's care file and persist as capacity changes — the late-stage resident may not remember setting preferences, but the preferences still govern the system's behavior. This respects the resident as author of their own story even as authorship becomes increasingly distributed.
See Ambient Capture in Practice
Ambient story capture is the infrastructure layer that turns long-term memory care from a slow-decline story-loss machine into a slow-weaving story-preservation system. If your funeral home partners with even two memory-care facilities, ambient capture is a meaningful differentiator competitors cannot easily match without the privacy and threading architecture to support it. Book a facility-demo visit — we will tour a partnered memory-care community running the system, walk through the staff review workflow with you, and show you what three months of ambient capture looks like for a single resident's tapestry compared to a matched resident without ambient capture running. The visit runs four hours and covers the consent ladder, the on-device processing stack, the staff review dashboard, the resident preference interview, and the privacy audit log your facility partner can show their compliance officer.
Firms that move forward receive a joint implementation engagement where our deployment team partners with the facility's operations lead to stand up ambient capture in two resident suites as a proof zone. The proof-zone engagement runs 90 days, includes weekly sync calls, and ends with a comparison report that quantifies fragment capture against the matched control suite. Most facility partners move to full-wing deployment within four months of the proof-zone outcome. Bring your director of partnerships, one memory-care administrator, and a family advisory representative — the visit produces an aligned decision framework across all three stakeholder groups.