Future of Wearable Biometric Capture for Perinatal Memorial Building
The Invisible Archive Most Pregnancy Loss Memorials Never Touch
A mother who wore an Oura ring across her pregnancy and lost her son at 31 weeks described the strange experience of scrolling back through her biometric data months after his funeral. Her resting heart rate had been climbing. Her sleep patterns had shifted. Her body had carried a record of his presence, written in physiological signatures, and that record still existed in an app she now avoided opening. She wanted the data. She also did not know what to do with it.
The Oura pregnancy insights research documenting resting heart rate increasing approximately 10 bpm by week 32 establishes that consumer wearables capture meaningful gestational signatures. The Nature study tracking biometrics of complete pregnancy across 10,318 users demonstrates that wearables can capture an entire pregnancy as a coherent dataset. A systematic review of wearable sensors for maternal health confirms the breadth of biometric data now available to pregnant users.
The gap is not data availability. The gap is memorial integration. When a pregnancy ends in loss, the biometric archive typically either sits unprocessed in a consumer app or gets deleted in an act of avoidance. No memorial workflow currently helps families extract, interpret, and integrate these biometric signatures into remembrance practice. The wearable fetal movement detection research documents how biometric capture extends to fetal patterns, making the potential memorial archive even richer.
The StoryTapestry Framework for Wearable Biometric Memorial Integration
StoryTapestry approaches biometric data the way a master weaver approaches an archive of hand-spun thread left by an earlier weaver: precious, abundant, requiring careful sorting, and beautiful when woven into the right pattern. The framework treats wearable data as a distinct memorial modality alongside photographs, voice, and written reflection, with its own capture, processing, and preservation protocols.
Four biometric data categories matter for perinatal memorialization. First, maternal biometrics across pregnancy: resting heart rate, heart rate variability, sleep architecture, body temperature. Second, fetal biometrics where captured: fetal heart rate patterns, movement patterns, and in specialized clinical contexts wearable cardiotocography data, which can be paired with audio waveform keepsakes to create multimodal prenatal memory artifacts. The Northwestern research on wireless sensors for pregnancy that outperform current technology documents expanding fetal capture capability. Third, context biometrics: partner heart rate during co-regulation, sibling activity, ambient household sleep data. Fourth, clinical biometrics shared by the care team, including NICU monitor data when death occurs in intensive care.
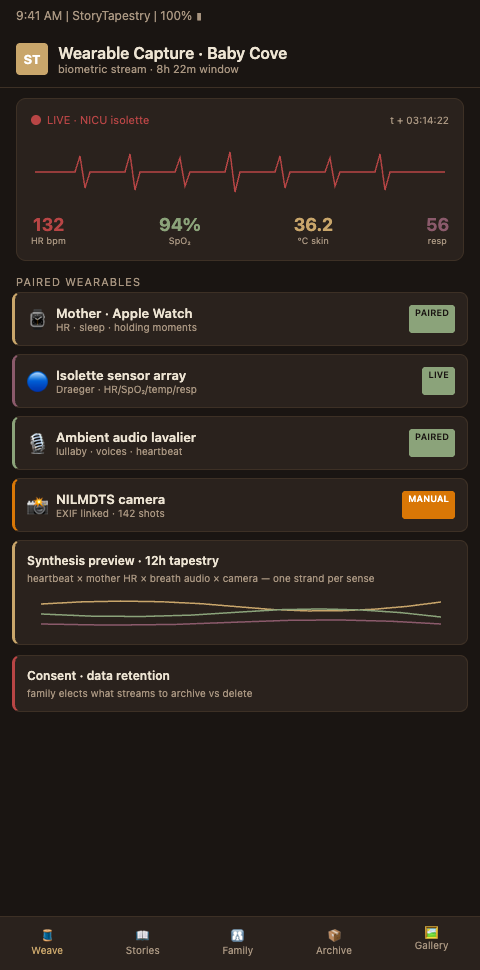
The platform's biometric integration pipeline operates in three stages. Stage one is consented data import from Apple Health, Google Fit, Oura, Garmin, and hospital EMR systems. Parents grant specific scope access to the platform and can revoke access at any time. Stage two is trauma-informed processing that produces visual artifacts without forcing parents to confront raw data they may find overwhelming. A resting heart rate timeline can be visualized as a flowing ribbon with each week color-coded. A sleep pattern across 31 weeks can be rendered as a mosaic. Stage three is tapestry integration where biometric artifacts become threads in the full memorial, annotated by the parent with reflections, memories, and context.
The tapestry metaphor holds because biometric data is not a single thread. It is an entire skein that weaves through every other thread. When the mother's resting heart rate line is displayed alongside her written entries, photographs, and audio clips, each thread reinforces the others. The ribbon of elevated heart rate becomes the physical substrate against which other memories sit. The systematic AI-enabled wearable sensor review for fetal detection suggests future capability where pattern recognition highlights specific moments in the biometric timeline, such as the first night the mother's sleep shifted in response to fetal circadian patterns.
The audio pairing with biometric capture is powerful. A mother can overlay her recorded lullaby on top of her heart rate variability timeline from the same weeks. The audio waveform keepsakes pipeline integrates with biometric visualization to produce multi-dimensional artifacts. For families participating in therapeutic memorialization outcomes research, biometric integration adds a quantitative dimension to meaning reconstruction work that complements traditional narrative approaches. The broader technology context connects to AI memorial technology developments across demographic domains.
The clinical interpretation layer matters more than the data ingestion layer. A mother looking at thirty-one weeks of resting heart rate data does not need a chart; she needs a bereavement-literate clinician who can sit with her and narrate what the chart shows. "Your resting heart rate climbed about eleven beats per minute between week eighteen and week thirty. That is what carrying a baby does to a body. Your body remembered him." This kind of narration cannot be automated. It requires a clinician who understands both the physiology and the emotional weight of the data, and who can present the numbers as evidence of the baby's presence rather than as clinical metrics. Hospital programs that deploy biometric memorialization without clinical interpretation training leave mothers staring at charts they cannot read, which is worse than not extracting the data in the first place.
The second infrastructure need is family control over granularity. Some parents want the week-by-week detail; some want only the high-level arc; some want only specific moments — the first night sleep shifted, the week the heart rate stabilized, the final forty-eight hours before loss. StoryTapestry supports granularity controls that let the parent choose which resolution of biometric data appears in the tapestry without deleting the underlying archive. A mother who initially wants only high-level arcs may, three years later, want to explore the week-level detail. The archive preserves both possibilities. Programs that force a one-time granularity choice at the moment of loss lock families into a resolution they may regret.
The third consideration is biometric data coming from the partner or other family members. A partner's Apple Watch data across the pregnancy may show sympathetic shifts that parallel the mother's biometric trajectory — synchronized stress responses, altered sleep on nights the baby was active, heart rate spikes during hospital visits. With the partner's consent, this data can be woven into the shared tapestry as evidence that the partner's body was carrying the pregnancy alongside the mother's in ways that are not usually acknowledged. This extends memorial capture to family members whose grief is often treated as secondary, and gives fathers and non-gestational partners a physiological thread in the memorial that validates their embodied experience.
Advanced Tactics for Ethical Biometric Memorial Integration
Wearable biometric memorialization requires tactical precision because the data is sensitive, the bereavement context is raw, and the technical infrastructure is still evolving. Four advanced tactics separate responsible implementation from reckless data exploitation.
Build consent that anticipates future choice. Biometric data extracted at the time of loss may be wanted immediately by some parents and overwhelming to others. The consent framework should allow parents to extract the data for preservation without requiring immediate processing or visualization. A parent can say "extract my pregnancy biometrics into my tapestry archive, but do not display them to me yet." Six months later, in a clinical session, the parent may choose to activate visualization. Consent that anticipates temporal shift matters more than consent that presumes immediate readiness.
Design trauma-informed visualization defaults that align with broader therapeutic memorialization outcomes research on clinically integrated memorial interventions. A resting heart rate timeline that abruptly terminates at the loss date is jarring. The default visualization softens the termination with a gradient, labels the transition in neutral clinical language, and allows the parent to choose how much of the post-loss period is rendered. The NICU emotional health research documenting long-term depression, anxiety, and PTSD risk reminds us that memorial infrastructure affects emotional health for years. Default design choices shape engagement outcomes.
Coordinate with clinical data partners. When NICU monitor data is part of the biometric archive, the hospital must release it through a structured data partnership with appropriate HIPAA compliance. StoryTapestry's clinical partnership framework includes BAAs, limited use agreements, and audit trails that make clinical biometric release defensible rather than improvised.
Plan for device obsolescence. The Oura ring of 2026 may not be the wearable of 2036. Biometric memorial archives must be format-portable so that the tapestry survives device transitions, a challenge that parallels the long-horizon data stewardship work behind AI memorial technology for veteran families. The platform's archival layer normalizes biometric data to open formats at capture rather than preserving vendor-specific files that may become unreadable.
Establish clinical team boundaries around biometric interpretation. Bereavement coordinators are not typically trained to interpret heart rate variability data or sleep architecture, and the temptation to over-interpret biometric patterns can produce inaccurate narratives that the family then carries for years. Programs that deploy biometric memorialization should partner with maternal-fetal medicine specialists, sleep medicine physicians, or exercise physiologists who can review the biometric narratives before they are finalized in the family's tapestry. A narrative that says "her heart rate was elevated because she was stressed" is often wrong; the correct narrative may be "her heart rate was elevated because carrying him increased her resting metabolic demand by approximately 15%." Clinical accuracy matters because the family will quote the narrative to each other and to future clinicians for years.
Coordinate with academic research partnerships that study biometric signatures in pregnancy. Several research groups are actively cataloging biometric patterns across pregnancy and pregnancy loss, and participation in these studies can add scientific context to a family's biometric memorial. A mother whose biometric data is included (with consent and de-identification) in a research cohort studying heart rate variability across pregnancy loss may receive, as part of her participation, a contextual report that compares her trajectory to cohort norms. The report is not a diagnosis; it is scientific context that can be integrated into the tapestry as a research thread. This positions the family's biometric memorial as part of a larger scientific conversation about pregnancy and loss, which some families find deeply meaningful.
Handle subsequent pregnancy biometric continuity. A mother who lost her previous baby and now carries a subsequent pregnancy typically wears the same Oura ring or Apple Watch. Her biometric data will inevitably be compared to the previous trajectory. StoryTapestry supports overlay views that can be shown, hidden, or toggled at any gestational week the mother chooses. Some mothers find the overlay comforting; others find it unbearable. Both responses are correct, and the architecture supports both.
Integrate Biometric Memorial Capture Into Your Bereavement Program
Hospital bereavement programs that want to extend memorial capture beyond photographs and voice recordings can pilot StoryTapestry's wearable biometric integration module with a cohort of consenting families. The module handles consent infrastructure, data import from consumer wearables and hospital EMR systems, trauma-informed visualization, and tapestry integration. Our clinical partnerships team supports the biometric pilot with ethics framework, consent language, and outcome measurement design.
Request a biometric integration consultation to map how wearable data becomes memorial input for the families your program serves in the decade ahead. The consultation includes a review of your current consent infrastructure, an assessment of your clinical partnerships for biometric interpretation, and a recommended pilot design with a cohort of ten to fifteen consenting families across six months. The pilot produces a consent framework reviewed by your compliance office, a clinical interpretation protocol developed with your maternal-fetal medicine team, and a set of family-reported experience measures that quantify whether biometric integration adds meaning or adds distress.
Bring your bereavement coordinator, a representative from your compliance office, and a maternal-fetal medicine specialist to the consultation. Biometric memorialization sits at the intersection of bereavement care, data ethics, and clinical interpretation, and the implementation needs all three perspectives from the beginning. Programs that defer any of the three produce pilots that stall — either because the consent framework fails compliance review, or because the biometric narratives are clinically inaccurate, or because the families find the visualizations more painful than helpful. The three-perspective consultation avoids these predictable failures.