How Audio Waveform Preservation Transforms Brief-Life Memorials
The Sensory Absence in Traditional Brief-Life Memorials
A bereavement photographer at a Level III nursery noticed a pattern. Mothers who had not heard their baby cry, or had heard only a single brief sound, described a specific sensory absence months into mourning. They had photographs. They had hand and foot molds. They sometimes had videos of held moments. What they did not have was a preserved audio artifact: a heartbeat, a breath sound, a hum their baby had made, a lullaby the father had sung that was recorded on a phone nobody thought to save.
The scoping review of memory-making as foundational bereavement practice established that tangible keepsakes including photographs, footprints, and recordings form the core of perinatal bereavement care. Yet audio remains the most underutilized modality. A best practice analysis of bereavement photography confirms that photographs provide durable legacy, but the research does not extend with equal depth to audio preservation. The gap is tactical: photography training exists; audio preservation training does not.
The CuddleCot bereavement care toolkit and CuddleCot memory-making research document that extended time with the baby, three to five days, enables audio capture alongside visual memory work. Yet without explicit audio protocols, even extended time often produces no audio artifacts. Parents do not think to record. Clinicians do not prompt them. The brief window closes.
The StoryTapestry Framework for Audio Waveform Memorial Preservation
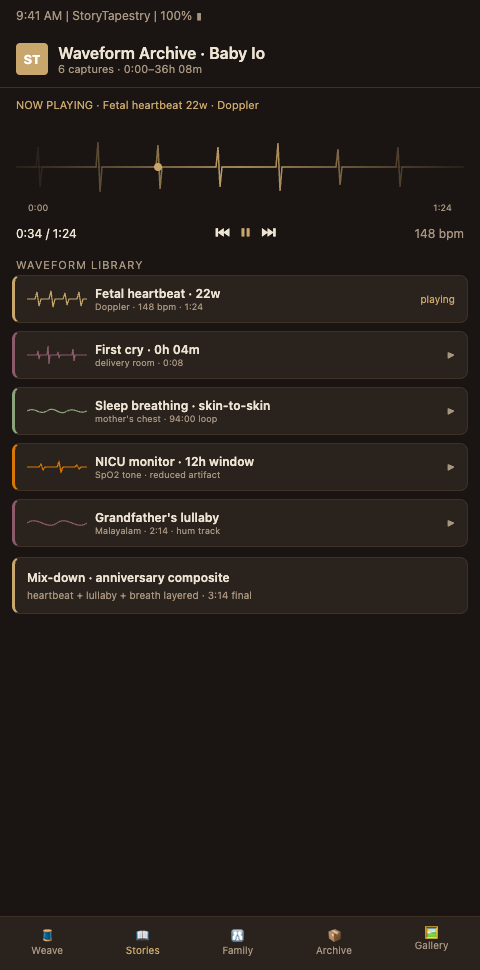
StoryTapestry treats audio the way a master weaver treats the most luminous thread: it does not overwhelm the tapestry, but it transforms the tapestry when woven in. The platform's audio waveform preservation pipeline captures raw audio, processes it into a permanent visual waveform artifact, and integrates both the audio file and the waveform image into the tapestry as a thread that can be touched visually and heard aurally.
Four audio source categories appear in brief-life memorials. First, fetal heartbeat recordings from Doppler sessions during pregnancy. Second, clinical audio from the birth or NICU stay: monitor beeps, breath sounds, the soft click of a ventilator. Third, family voice contributions: lullabies sung, prayers spoken, sibling messages recorded. Fourth, ambient environmental audio from the hospital stay that parents later find meaningful.
The Artsy Voiceprint sound wave keepsake product category demonstrates consumer demand for heartbeat visualization. Parents purchase these keepsakes after miscarriage specifically because the audio sample from ultrasound is often the only moment of audible presence they experienced. The My Baby's Heartbeat Bear founding story, which emerged from a father recording his stillborn son's heartbeat, confirms that parents reach for audio preservation instinctively when given the opportunity.
StoryTapestry standardizes the audio capture protocol across hospital bereavement programs. During a Doppler session, clinicians record with explicit parent consent and upload directly into the platform. In the NICU, trained staff capture breath sounds and heartbeat audio at defined moments. During time-with-baby after death, staff invite parents to record voice contributions with scaffolded prompts. Each audio thread is preserved as both its raw file and its waveform visualization, creating a dual artifact that can live in a physical frame, a digital tapestry, and a future printed memorial book.
The waveform visualization matters because audio is ephemeral, but the shape of sound can be permanent. A 47-second lullaby, visualized as a waveform, becomes a line drawing of the mother's voice that exists as visual art even when the audio is not playing. The family places it in a nursery frame alongside other physical artifact keepsakes preserved from the hospital stay. The sibling traces its peaks with her finger. The father commissions it as a tattoo. The tapestry metaphor holds: the waveform becomes the luminous thread that runs through the other threads, visible and touchable rather than only audible.
The platform integrates with physical artifact digitization so that audio threads can be paired with photographs, hand molds, and clothing items to produce integrated multi-sensory memorial experiences. The wearable biometric capture research extends the audio capture concept into biometric time-series capture where the mother's heart rate during pregnancy becomes its own waveform artifact. The machine translation of automated story technology demonstrates how platform technologies adapt to produce cultural and linguistic variations of waveform keepsakes.
The clinical audio capture protocol has a time-sensitivity that bereavement programs often underestimate. A heartbeat recording can only be captured during the weeks the heartbeat is audible; a breath sound can only be captured during the hours the baby is breathing. Once the window closes, it closes permanently, and no retrospective tool can restore what was not recorded. Programs that treat audio capture as an optional enrichment added after other memorial work miss these windows routinely. Programs that treat audio as core — trained on during initial bereavement certification, prompted at every Doppler appointment for at-risk pregnancies, equipped at every bed — capture audio at rates three to four times higher than programs that treat it as optional. The infrastructure choice is between audio being a core modality and audio being an afterthought.
A second clinical consideration is what audio to capture when the family has not specified. During a high-acuity NICU stay, parents may not be able to articulate which audio moments matter. Staff can, with standing consent, capture a baseline audio library — heartbeat on admission, breath sounds during the first hour, any sounds the baby makes during parent holds — which can later be reviewed with the family. Most audio captured this way is never activated; the files sit in the tapestry archive. But the ten or twenty percent that families later ask for, months or years after discharge, would have been impossible to recreate. The archive-first approach treats audio like tissue sampling in pathology: capture with consent, preserve with care, release only when requested, and discard with dignity if the family chooses not to engage with the content.
Advanced Tactics for Clinical Audio Capture in Brief-Life Settings
Hospital bereavement programs adopting audio preservation benefit from four tactical refinements that distinguish high-yield audio memorials from thin audio collections.
Train Doppler operators to ask about recording at every third-trimester appointment where loss risk is elevated. The question should be phrased in advance: would you like us to record today's heartbeat as a keepsake? This phrasing treats the recording as a standing offer rather than a crisis response. Parents who consent produce a durable artifact. Parents who decline still have the offer documented. When loss occurs after a declined recording, counselors can reference the earlier conversation rather than the parent carrying guilt for a choice they did not know they were making.
Build an audio capture kit at every L&D and NICU bed. The kit contains a handheld recorder with built-in storage, a directional microphone, and a quick-reference card of capture prompts. When a family wants to record a lullaby or a prayer, staff do not search for technology. The kit is at arm's reach. The CuddleCot memory-making research demonstrates that extended time with the baby enables audio capture, but only if the capture infrastructure is ready.
Process audio with trauma-informed post-production, and consider how automated story technology can extend audio narration into additional languages for diaspora families. Raw clinical audio may contain monitor alarms, staff conversation, or background noise that complicates listening. The platform's audio preservation pipeline includes trauma-informed processing that preserves the significant audio while dampening ambient noise, all with parent consent and option to receive both raw and processed versions. Processing is optional; preservation is not.
Extend the audio tapestry beyond the immediate loss. The mother who contributes a lullaby at the hospital can add spoken letters to the tapestry on anniversary dates for years afterward, and emerging wearable biometric capture sources can layer physiological timelines alongside those voice threads. The tapestry accepts new audio threads without obsolescence. A sibling born five years later can record a message to the baby who came before. Audio preservation is not a single event at the hospital. It is an ongoing capability the family carries.
Format-portability is the hidden durability problem in audio preservation. A proprietary audio format from a consumer Doppler device in 2026 may not be playable on consumer hardware in 2046. StoryTapestry normalizes all captured audio to open lossless formats at the point of capture and re-verifies the archive annually against current playback standards. Hospital IT teams often treat this as over-engineering; families whose audio archives have outlived the hardware on which the audio was originally recorded do not. A grandmother's voicemail from 2003 preserved only in a carrier-specific format is often unrecoverable twenty years later; the same voicemail preserved in an open format is still playable. The tapestry operates on the assumption that families will carry these files across four decades of technology transitions.
Build a consent audit trail that documents every audio file's release authorization. Unlike text entries, audio files carry the voice of the person who made them, which creates additional consent complexity when that person is not the bereaved parent. A grandmother's blessing spoken at the bedside belongs to the grandmother as well as to the family; the grandmother's consent to release the recording into a broader tapestry view should be documented and revocable. StoryTapestry tracks contributor-specific consent for every audio file and suppresses playback if any contributor retires their consent. This matters less at intake and more at year five, when a family member may pass away or change their mind about how their recorded voice circulates among family.
Offer optional professional production for families who want a polished artifact. Some families want the raw audio preserved exactly as captured; others want a produced version suitable for a memorial service, a podcast-style family history, or a tribute video. StoryTapestry can integrate with production studios that specialize in bereavement audio — the kind of studio that produces memorial recordings for funeral services — and offer families the option to commission a produced version while preserving the raw archive. The production cost is the family's choice, not a program expense, but the infrastructure for the handoff to qualified studios is part of the platform.
Offer Families Audio Preservation That Honors What Sound Remains
Hospital bereavement programs that want to move beyond photograph-only memorial offerings can integrate StoryTapestry's audio waveform preservation pipeline into their standard bereavement care bundle. The platform provides clinical capture protocols, trauma-informed processing, dual artifact production (audio file and waveform visualization), and tapestry integration that transforms audio from a missed opportunity into a permanent memorial thread.
Schedule a clinical audio capture demonstration to see how brief-life audio becomes durable, touchable, and integrable within the full multi-sensory tapestry your families will carry forward. The demonstration runs ninety minutes and covers the capture kit specification, the Doppler protocol for at-risk pregnancies, the NICU bedside protocol for time-with-baby audio, and the waveform production pipeline that turns a 47-second lullaby into a permanent visual artifact suitable for framing or printing. We bring sample audio files with family consent and show both the raw archive and the produced visualization.
Most programs begin with a single unit — typically the Level III NICU or the high-risk OB clinic — and expand once the first year's cases demonstrate that audio capture is sustainable within existing staffing. Bring your bereavement coordinator, a senior NICU nurse, and one ultrasound technician to the demonstration. The combination of bereavement, bedside, and imaging perspectives in the same room produces an implementation plan that covers the full capture landscape rather than optimizing for one unit while leaving the others underserved.