Therapeutic Outcomes of Digital Memorialization in Pregnancy Loss Recovery
The Therapeutic Gap Between Ritual Grief and Clinical Care
A bereavement counselor at a tertiary obstetric unit sees roughly 180 families per year after pregnancy loss. She has access to referrals for individual therapy, support groups, and medication management. What she does not have in her standard toolkit is a therapeutic intervention that patients can carry between sessions, activate at 3am, and share with a partner who refuses to attend counseling. For her patients who cannot afford weekly therapy or live 90 minutes from the nearest grief specialist, the therapeutic gap is unbridgeable with her current resources.
The web-based bereavement care review documenting large effects for PTSD (g=0.86) and moderate effects for grief revealed that digital interventions are not a pale substitute for in-person therapy. They produce clinically significant outcomes across populations. A randomized controlled trial protocol for the Living with Loss online program showed that internet-based bereavement programs reduce psychological distress post-program and at follow-up. The question for hospital bereavement programs is not whether digital memorialization works therapeutically. It is how to deploy it with the rigor that produces outcomes.
Most digital memorial offerings in the market are not therapeutic. They are template-driven tribute pages designed for public sharing. They do not incorporate meaning reconstruction frameworks, innovative moments tracking, or expressive writing protocols. Families use them for announcement and ritual, then return to clinical isolation between appointments.
The StoryTapestry Framework for Evidence-Based Memorial Therapy
StoryTapestry treats digital memorialization as a weaving practice with clinical scaffolding. The tapestry metaphor matters because therapeutic memorialization is not a single act but a repeated return. Each visit to the tapestry adds a thread. Over weeks and months, the tapestry thickens. The act of weaving becomes therapy in itself, grounded in evidence that meaning reconstruction reduces complicated grief symptoms.
Neimeyer's meaning reconstruction framework, documented across decades of grief research on meaning reconstruction and mourning, establishes that bereaved individuals heal through constructing meaning about the loss, the deceased, and the self. StoryTapestry operationalizes this framework through three thread types: narrative threads (what happened and when), meaning threads (what this moment revealed about who our baby was), and self-revision threads (how I am different because of this life). Each thread type maps to a specific therapeutic mechanism. Narrative threads stabilize traumatic memory. Meaning threads support integration. Self-revision threads enable identity reconstruction after loss.
Innovative moments tracking, a concept grounded in constructivist grief therapy that documents meaning reconstruction through narrative, shows that therapy succeeds when clients articulate moments of reflection, reconceptualization, and performing change. StoryTapestry invites contributors to mark specific entries as innovative moments, which allows both the bereaved parent and a treating clinician to identify therapeutic progress through the tapestry's growth rather than through session recall alone.
Expressive writing, supported by a meta-analysis showing moderate effects for grief, is scaffolded within the platform through trauma-informed prompts. Parents are not handed a blank screen. They are offered graduated prompts: sensory prompts for those who cannot access emotion directly, reflective prompts for those ready for feeling language, and meaning prompts for those integrating the loss into their broader life narrative. The digital storytelling research documenting bonding creation for bereaved families confirms that structured digital storytelling produces measurable bonding and coherence outcomes.
The 24-hour access benefit matters therapeutically, especially when paired with multi-perspective grief healing approaches that invite contributions from multiple family members. A rapid review of online bereavement support demonstrated that asynchronous access allows engagement during the 3am grief spikes that conventional therapy cannot address. When a bereaved mother wakes at 4am unable to return to sleep, she can open the tapestry, add a thread, read her partner's entries, and find structured comfort that meets her in the moment. This access pattern is not a convenience. It is a clinical feature.
For hospital bereavement programs, integrating therapeutic digital memorialization requires three commitments: clinical supervision, outcome measurement, and clinician literacy. Clinical supervision means a grief-trained clinician reviews tapestry engagement at 2, 6, and 12 weeks and flags concerning patterns. Outcome measurement means standardized measures administered at baseline, 12 weeks, and 12 months. Clinician literacy means counselors integrate tapestry entries into session work, referring to specific threads and inviting the client to add threads that surfaced during the session.
This framework pairs naturally with emotional impact measurement protocols that quantify whether memorial engagement correlates with reduced grief complications. It also connects to the multi-perspective grief healing research base, because solo memorial engagement produces different outcomes than shared family engagement. Programs that already use oral history techniques for veteran memorials can transfer those interview skills to perinatal contexts.
The three-thread typology — narrative, meaning, self-revision — gives grief-trained clinicians a structured way to read a tapestry as a therapeutic document rather than a sentimental one. A clinician who looks at a tapestry and sees eighteen narrative threads, four meaning threads, and zero self-revision threads at six months post-loss has useful diagnostic information: the parent is stabilizing traumatic memory successfully but has not yet entered integration work. This reading is not a deficit; it tells the clinician where to focus the next few sessions. Conversely, a tapestry with three narrative threads and fifteen self-revision threads at six weeks may signal that the parent is running ahead of their own traumatic memory processing, skipping the stabilization work and rushing toward identity reconstruction before the foundation is set.
Reading tapestries is a clinical skill that can be taught, and the platform supports training through case libraries of de-identified tapestries with clinician annotations.
The platform's therapeutic value also extends to partners and family members who would never enter individual therapy on their own. A father who declines counseling referral may still contribute to the tapestry and, through that contribution, encounter graduated prompts that invite reflection without framing it as treatment. Over weeks and months, his contributions accumulate into a record his treating clinician (who is typically working with the mother) can reference when the couple eventually meets for a joint session. The tapestry becomes a bridge into clinical engagement for family members who would otherwise remain outside the therapeutic frame. This is not manipulation; it is scaffolding. The father is always told what the tapestry does and what his clinician can see, and he retains full control over what is shared with whom.
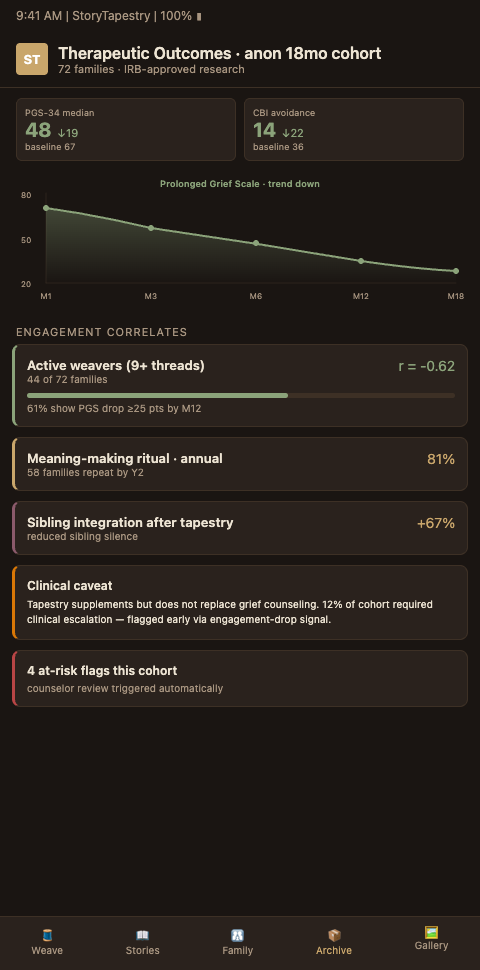
Advanced Tactics for Clinically Integrated Memorial Interventions
Hospital bereavement programs that move from supportive memorialization to therapeutic memorialization require four advanced tactics.
First, credential the intervention inside your clinical care pathway. When StoryTapestry engagement appears in the EMR as a documented intervention with tracked dosage and outcomes, it moves from a kind gesture to a clinical tool. Insurance panels, institutional review boards, and health system quality committees all respond differently to interventions with dosage and outcome documentation than to adjunct wellness offerings.
Second, pair therapeutic memorialization with a primary clinician relationship. Pure self-guided digital intervention produces smaller effects than clinician-supervised digital intervention. The tapestry augments the counselor. It does not replace her. When parents know their counselor reads their tapestry between sessions and will gently reference specific entries, engagement depth increases substantially.
Third, build multi-modal expressive capacity. Some parents write. Some record voice, using oral history techniques adapted from veteran memorial practice. Some upload photographs and annotate them. Some draw and upload scans. Therapeutic efficacy depends on matching modality to parent preference. The tapestry should invite every modality and preserve it with equal archival quality.
Fourth, track intergenerational access. Parents of pregnancy loss are often already parents of living children, or become parents of subsequent children. The tapestry becomes part of family history. When a living older sibling, at age 12, asks about the baby who came before them, the tapestry becomes the artifact that answers. Therapeutic memorialization extends its clinical utility across decades.
Fifth, supervise adverse event monitoring as rigorously as you would in any clinical trial. Therapeutic memorialization can occasionally destabilize a parent who encounters content they were not ready for, or who engages at a pace that exceeds their capacity for integration. The platform includes adverse engagement patterns — sudden engagement cessation after heavy early use, engagement spikes at clinically implausible hours that suggest crisis rather than reflection, repeated return to a specific thread without new contributions suggesting stuck processing — and surfaces these patterns to the supervising clinician for outreach. The outreach is not punitive; it is clinical. A bereavement counselor who reaches a parent within 48 hours of an adverse engagement pattern often prevents a crisis that would have resulted in an emergency department visit three weeks later. This monitoring is the feature that moves the platform from a wellness app to a clinical intervention.
Sixth, align the intervention with existing perinatal care handoffs. A bereaved mother often re-enters the obstetric care system within one to three years for a subsequent pregnancy. Her prenatal team typically has no structured awareness of her previous loss beyond a one-line entry in her chart. Therapeutic memorialization done well produces a documented tapestry that, with the mother's consent, can be surfaced to her prenatal team at key gestational milestones — particularly the gestational week at which she lost her previous baby. Obstetric teams who know to expect heightened anxiety at that week, and who can reference the previous tapestry in conversation if the mother initiates it, provide markedly better subsequent-pregnancy care than teams who have no awareness of the earlier trajectory.
Seventh, integrate with patient-reported outcome measurement infrastructure. Many health systems already collect PROMIS or similar standardized patient-reported outcomes. Therapeutic memorialization's grief outcome data can be integrated into these existing systems rather than running in parallel. This integration requires upfront IT work but produces two benefits: the grief outcome data becomes part of the system's standard quality metrics, and the memorialization program gains protection during budget cycles because its outcomes are visible in the reports leadership already reads.
Partner With a Therapeutic Memorial Platform Built for Bereavement Programs
Hospital bereavement programs that want to offer families more than supportive ritual can adopt StoryTapestry as a clinically scaffolded therapeutic intervention. We built the platform in partnership with grief-trained clinicians, perinatal bereavement specialists, and families who had navigated loss.
Request a clinical integration consultation with our team to map how the platform integrates with your existing care pathway, what outcome measures align with your program, and how to credential the intervention within your health system. The consultation includes a review of your current clinical supervision capacity, your outcome measurement infrastructure, and your counselor literacy around digital tools. Most programs that transition from supportive memorialization to therapeutic memorialization need six to nine months of preparation before they can deploy the platform as a clinical intervention: clinicians need training on reading tapestries therapeutically, outcome measurement instruments need to be added to the intake workflow, and the EMR credentialing needs to be built.
Therapeutic memorialization is available to your families. The question is whether your program is ready to deploy it. We work with programs at any stage of that readiness — from hospitals with no current memorial program who want to build a therapeutic model from scratch, to programs with mature supportive memorialization that want to add clinical scaffolding, to academic centers ready to run a formal research protocol. Bring a bereavement coordinator, a licensed grief clinician, and one representative from your quality and safety team to the consultation. The combination of clinical, operational, and quality perspectives in the same room produces better implementation plans than any of those roles produces alone.