Building Trust with Memory Care Families During Story Gathering
The Trust Deficit in Memory Care Bereavement
A 2024 NFDA study surveyed 1,104 consumers and found that only 16% correctly understood the meaning of "memorial service," with similar gaps across the professional vocabulary funeral directors use every day (PRWeb - NFDA Communication Gap Study). The gap widens with memory care families who are simultaneously processing the death, exhausted from years of caregiving, and navigating their own complicated grief from anticipatory loss that preceded the physical death. The NFDA's companion guide frames this as a research-backed communication bridge that the profession has historically lacked (NFDA - When Words Matter Guide).
Memory care families arrive at arrangement conferences with specific trust fragilities that generic bereavement training does not address. The primary caregiver daughter spent the last four years being second-guessed by siblings about medical decisions and now braces for similar second-guessing about memorial decisions. The husband who managed his wife's decline feels guilty about every moment he was not present and hears "tell me about her" as an audit of his attentiveness. A mixed-methods review of funeral practices confirms that family interpretation of the funeral director's communication style strongly predicts bereavement mental health outcomes (PMC - Funeral Practices Bereavement Mental Health). Families who feel judged in the first conference contribute superficial stories afterward, and the resulting memorial feels hollow.
Weaving Trust Into the Story-Gathering Tapestry
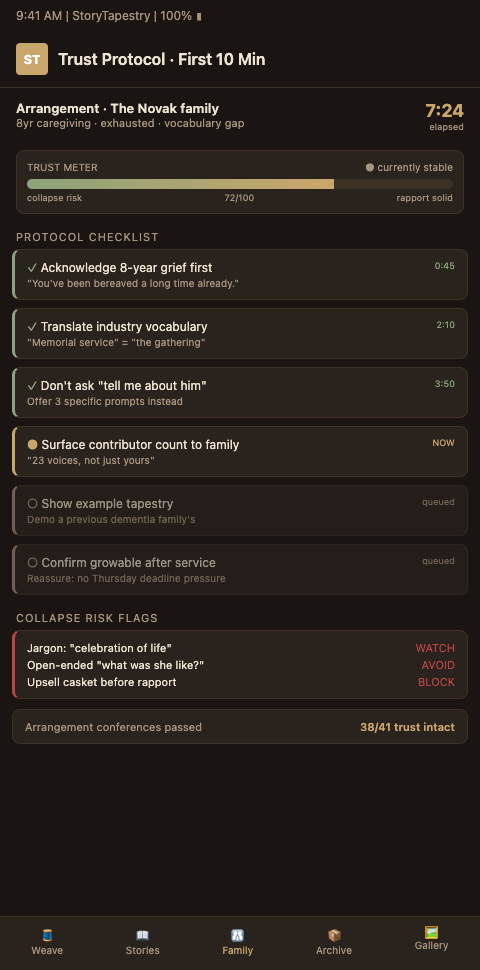
StoryTapestry's intake workflow is built on the premise that trust is itself a thread in the memorial tapestry, not a preliminary step before the "real" work begins. The tapestry metaphor matters because a memorial woven without the family's confidence will show its weak threads at the service; every dementia family has a finely tuned detector for whether the funeral director actually listened or processed them through a template. Japanese survey research on funerals mediating grief shows that psychosocial outcomes correlate strongly with families feeling that the service authentically reflected the deceased and their circle (ScienceDirect - Funerals Psychosocial Impact).
Trust-building in memory care bereavement begins with vocabulary calibration. The Kates-Boylston analysis of the NFDA research argues that funeral professionals must adjust language based on what families actually understand, not what the profession prefers (Kates-Boylston - Speaking the Language of Healing). StoryTapestry's family-facing intake avoids professional jargon by default and allows directors to insert specific terms only after confirming the family recognizes them. A family who says "funeral" when they mean "memorial" should not be corrected; the system captures their preference and uses it throughout.
Empathy dimensions in bereavement support have been studied extensively. Research on empathy and bereavement support strategies distinguishes cognitive empathy (understanding the family's situation) from affective empathy (feeling their distress) from compassionate empathy (motivated action) (ResearchGate - Empathy and Bereavement Support). Memory care families respond especially to compassionate empathy demonstrated through logistical action: "I'll contact the memory care facility directly for the aide who knew her best; you don't need to make that call." StoryTapestry builds this action capacity into the workflow by pre-populating contact channels with the facility's staff directory, so the funeral director can make good on the offer without asking the family to locate numbers.
The ethics of difficult funeral conversations require transparency about what is happening and why (Elite Learning - Ethics in Funeral Services). With memory care families, this means naming the anticipatory grief support dimension directly: "Many families who cared for someone with dementia tell me they grieved the person they knew before the disease and then grieved again now. That's two different losses, and we can honor both." Families who hear their experience named correctly relax into the interview.
Trust building also requires explicit acknowledgment of the sibling tensions that dementia caregiving produces. The primary caregiver daughter who lived 12 minutes from her mother for the final six years has a different relationship with the deceased than the brother who flew in twice a year from Seattle. Both loved her. Neither loved her more. But the daughter has witnessed her mother's decline in a way her brother has not, and the arrangement conference often becomes the first time these imbalances surface publicly. StoryTapestry's contributor attribution structure treats each sibling's input as a thread with its own color rather than forcing the family to produce a single consensus account.
The daughter's description of her mother's final birthday party and the brother's description of their childhood Thanksgivings are both true, and the memorial that includes both reflects the full relational picture rather than flattening it to please the dominant voice. Directors who name this pattern early in the conference ("Each of you saw your mother from a different angle; we're going to collect all of those angles before we assemble anything") produce families that arrive at the service feeling heard rather than managed.
Advanced Tactics for Memory Care Trust Building
Three tactics separate funeral homes that build reliable trust from those that alienate dementia families in the first conference. First, structure the initial session as a listening appointment, not an arrangement meeting. Memory care families often need 40 minutes of narrative venting about the decline years before they can focus on memorial planning. Directors who try to push into logistics in the first 10 minutes consistently produce thin story material. StoryTapestry's intake tags the listening phase separately so directors can track when families are emotionally ready to begin formal story capture.
Second, address ethical story consent early and explicitly. Memory care families often carry guilt about representing a person who could not participate in their own memorial planning, and the unspoken question is whether the funeral director will notice or gloss over this tension. Naming it directly ("Your mother could not tell us herself what she wanted. We'll work to honor who she was, knowing she is not here to correct us.") builds trust that surface-level sympathy cannot.
Third, extend the intake surface area to facility staff and extended family through contributor network building. The primary caregiver daughter is often relieved when the funeral home reaches out directly to the memory care aides, hospice chaplain, or out-of-town cousins rather than expecting her to aggregate everything. The relief itself becomes trust. For memory care funeral homes, this requires infrastructure to manage many small contributions from many contributors, which is what StoryTapestry is built to do.
Fourth, track trust signals through the first conference with explicit observation rather than intuition. Directors who log what questions the family answered fully, what questions produced short answers, and what moments produced emotional openness build a trust map that informs the second conference. A family that shut down when asked about the final decline but opened up when asked about pre-diagnosis gardens should not be pushed back into decline material in the next session; the director should continue drawing from the receptive channel until the family indicates readiness. StoryTapestry's intake notes capture these observations as structured fields rather than free-text memory, so directors returning to a case after a weekend can resume with the family's trust state intact rather than starting over.
Fifth, protect the trust investment across staff transitions. Memory care funeral home directors take vacations, leave the firm, or rotate cases. A family who built trust with one director and then met a second director for the second conference experiences the transition as broken continuity unless the second director arrives already familiar with every detail of the first conference. StoryTapestry's case transfer workflow includes a mandatory briefing artifact that the incoming director reviews before any family contact, and the family's first interaction with the new director begins with explicit acknowledgment ("Sarah told me about the conversation you had last Tuesday about your mother's rose garden") so the trust transfers rather than resetting.
Let StoryTapestry Build Trust Infrastructure for Your Memory Care Partnerships
Funeral homes that serve memory care facilities reliably are distinguished by their ability to earn trust from exhausted, ambivalent, or guilt-burdened dementia families within a single conference. StoryTapestry provides the vocabulary calibration tools, empathy-action shortcuts, and distributed contributor workflows that make trust an operational feature rather than an aspiration dependent on any one director's charisma. Contact StoryTapestry to arrange a partnership consultation tailored to memory care funeral homes ready to elevate the trust experience of the bereaved dementia families your facility partners refer to you.
Pilot partner firms receive direct support from the StoryTapestry product team in calibrating the family-facing vocabulary to match their local community's language, training directors on the listening-first conference structure that separates the emotional venting phase from formal story capture, and setting up the facility staff contact shortcuts that let directors make good on empathy-action offers without asking grieving families to locate phone numbers. Your first ten memory care bereavement engagements on the platform receive concierge support with post-case review sessions that surface which trust signals your directors read accurately and which ones they missed, producing measurable improvement across the pilot cohort. Your feedback shapes the production release of the vocabulary calibration library, the sibling attribution structures, and the case transfer briefing templates that make trust survive staff transitions.
Schedule a consultation to discuss how your memory care funeral home can move trust from a charisma-dependent variable to an operational constant your facility partners can rely on for every family they refer.