Understanding Grief When Cognitive Decline Precedes Loss
The Problem with Death-Centered Grief Models
Most funeral home bereavement programs are built around the death as the grief onset point. That framework fails catastrophically for dementia families. According to a Taylor & Francis systematic review of anticipatory grief, the prevalence of anticipatory grief in dementia caregivers ranges from 47% to 80%. A separate PMC study of pre-loss grief in caregivers of DLB found 47-71% experience significant pre-loss grief. By the time these caregivers sit across from a funeral director, they have carried grief for years, and another funeral-service framework that treats them as newly bereaved feels hollow.
The clinical framing matters. PMC's theoretical model of dementia grief describes this experience as unique, prolonged, and with an unclear endpoint spanning 8-10 years. The APA's podcast on ambiguous loss with Pauline Boss traces the term to 1970s research: the person is physically present but psychologically altered, producing a grief that the culture has no ritual for. Funeral homes that arrive only at the physical death miss the psychological death that happened years earlier and often leave families feeling that the memorial service doesn't match the shape of their loss.
Weaving a Memorial That Honors Pre-Death Grief
The framework shift is treating the memorial tapestry as something that begins during active cognitive decline, not at death. StoryTapestry makes this literal: a family can open a tapestry when a loved one is diagnosed, contribute fragments across the care journey, and let the memorial evolve as the person does. The tapestry becomes a companion to ambiguous loss rather than a reaction to physical death. Each pre-decline fragment is a thread captured before it could fade, and each post-diagnosis observation preserves the person as they still are, including in their altered state.
Alzheimer's Association guidance on coping with grief describes how Alzheimer's caregivers cycle through denial, anger, guilt, and acceptance repeatedly as the disease progresses. A memorial tapestry that grows over years absorbs this cycle without forcing the family to produce a final narrative in the week after death. NIA guidance on coping with grief and loss emphasizes the value of grief counseling and support groups, and the tapestry extends that principle by giving the family a persistent, tangible artifact of their loved one that they can contribute to during the hardest stretches.
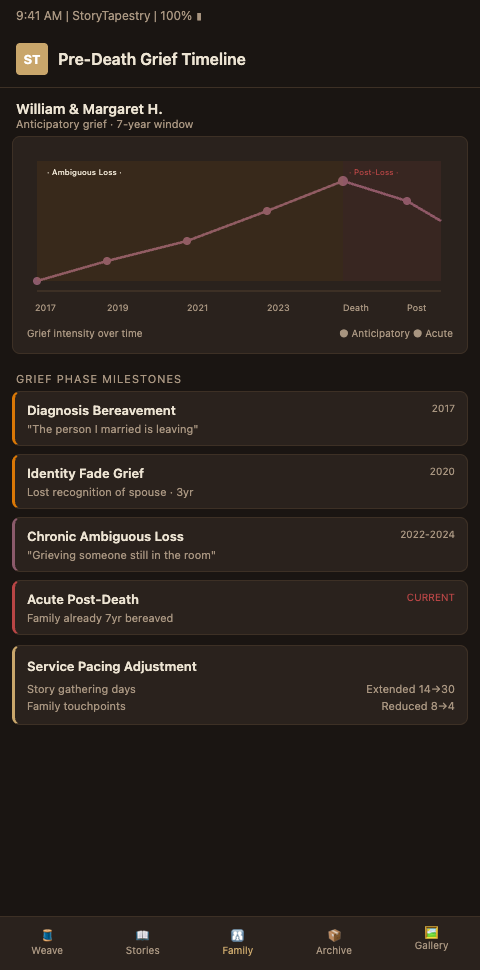
The Pre-Decline Proactive Gathering benefit matters most here. Families who open a tapestry early preserve the person's own voice, phrases, and self-narration. A voice memo from the year of diagnosis captures what will be lost within 24 months. Photos labeled by the person themselves carry context that will become unrecoverable. Pre-diagnosis memories are often the last opportunity for first-person contribution, and a tapestry that opens early captures them before the window closes.
Cognitive-Stage Sensitive Prompts adapt over time. Early-stage prompts invite the person to narrate their own life. Mid-stage prompts shift to caregivers capturing lucid moments and emerging routines. Late-stage prompts focus on sensory observations, musical preferences, and relationship texture with staff. The tapestry metaphor holds across stages because new threads continue weaving into the same fabric. This approach pairs naturally with ethical memorial assembly practices that address what to do when the person cannot consent to the memorial that will represent them.
Contradictory Memory Reconciliation carries unusual weight for pre-death grief. Family members often disagree about when the person "really" became unreachable. The tapestry preserves these disagreements as parallel threads, acknowledging that one sibling may have experienced the loss years earlier than another. Grief timelines in dementia simply do not match the standard bereavement expectations the industry was built around.
The contributor experience during a multi-year tapestry evolves as the person evolves. A son contributing in year one writes about his mother's recent cooking and her plans for the garden. By year four he is contributing about her repeated stories and the moments she still recognizes him. By year seven he is contributing about the color of her cardigan and the hymn she hummed during bath. Each era of contribution is different in tone, length, and emotional register, and the tapestry preserves all of them as threads woven into one memorial rather than forcing the son to produce a consistent voice across seven years of change. This honors the reality that grief during dementia is not a single event but a series of losses, each with its own accompanying record.
Advanced Tactics for Multi-Year Tapestries
The common mistake funeral homes make is offering only a post-death intake. Firms that build pre-diagnosis and mid-journey intake options see dramatically higher family satisfaction and deeper memorials. The practical rollout is a three-touch cadence: diagnosis touch (offer tapestry opening during family's first planning conversation), mid-journey touch (check-in at 18 months post-diagnosis), and late-stage touch (coordinate with hospice transition). Each touch offers tools and resources, not sales.
Edge cases worth scripting. Families where one member refuses to acknowledge the cognitive decline often reject pre-death memorial work. Leave the tapestry available but unpromoted until the family is ready. Families where multiple members hold conflicting timelines need routing so their threads do not collide in a way that reignites conflict. Families where the person with dementia is still capable of contributing need a consent flow that respects their fluctuating capacity without requiring legal guardianship determination for each entry. Families who open a tapestry early and then experience a rapid decline before they contribute substantially need gentle outreach, because the tapestry can become a source of guilt if not handled with care. The director's role includes reminding families that starting late is better than not starting, and that a thin pre-death tapestry still produces a richer memorial than a post-death blank page.
Scaling across a funeral home network requires staff training on grief vocabulary. Directors trained only on acute post-death grief often mishandle the mid-journey check-in and come across as transactional. Pair director training with facility-embedded social workers or chaplains who understand ambiguous loss as a clinical category. The investment pays off in referral volume and family loyalty, but it is an investment, not a quick wins program.
Measure program health with three signals: percentage of memorials opened before the physical death, average contributor count for pre-death vs post-death memorials, and family reports of tapestry use during active grief stretches. Firms with rising numbers on all three signals are doing the work correctly.
The clinical partnerships that make pre-death memorial work sustainable often live outside the funeral home's traditional relationships. Neurologists, geriatric social workers, memory care activity directors, and community-based ambiguous loss support groups all have patient contact during the pre-death grief window. A funeral home that builds referral relationships with these partners, not as marketing but as bereavement program extensions, becomes visible to families before crisis rather than after death. The investment is one coffee meeting per quarter with each partner, plus a shared protocol for introducing the tapestry concept when a family expresses readiness. Firms that build this network find their pre-death memorial volume grows organically rather than depending on post-diagnosis outreach the funeral home has to initiate.
Staff resilience matters for directors doing pre-death grief work. Walking alongside families for years before the death is emotionally heavier than post-death arrangement conferences, and directors who do not receive supervision or peer consultation burn out within two to three years. Build a monthly case-review group where directors can discuss the harder pre-death situations, a clinical consultation line for ambiguous loss questions, and explicit permission for directors to step back from specific families when their own grief is triggered. Firms that invest in staff resilience retain director talent, and retained directors are the operational backbone of any pre-death memorial program. The principle mirrors the handling of tangible grief artifacts in other niches where grief timelines fall outside standard bereavement expectations and directors need structured support to stay present for years rather than hours.
Build Memorial Tapestries That Honor Pre-Death Grief
Memory Care Funeral Homes on the StoryTapestry waitlist are among the first to pilot the diagnosis-onset memorial tapestry for Alzheimer's and dementia families. If your directors have watched families carry grief for years before a death and then felt their tools mismatch the shape of the loss, this workflow gives you structured pre-decline gathering, cognitive-stage sensitive prompts, and tapestries that evolve across the care journey. Reserve a pilot slot to help shape the three-touch cadence and director training for pre-death grief work in your region.
Pilot partners receive supervised onboarding for directors entering pre-death grief work, training modules on ambiguous loss vocabulary and the three-touch cadence, and assembly support for the first tapestries your firm opens at the diagnosis stage. The StoryTapestry product team works alongside your leadership during the first 90 days to adapt the workflow to your facility partnerships, your local referral networks, and the specific populations your firm serves. Your feedback shapes the production release of the three-touch cadence templates, the ambiguous loss prompt library, and the clinical partnership playbook that lets funeral homes build relationships with neurology practices and geriatric social workers. Reserve a pilot slot to move your memory care bereavement program from post-death intake only toward the multi-year model that families carrying dementia grief recognize as matching the actual shape of their loss.