Coordinating Multi-Site Story Collection Across Care Facilities
The Multi-Site Coordination Breakdown in Memory Care
Nursing home staff turnover averages over 100% annually in the United States, which directly disrupts continuity of care and story preservation across the patient's journey (PMC - Nursing Home Turnover Quality). A patient who moves from independent living to assisted living to memory care to skilled nursing typically leaves behind four separate charts, three life enrichment programs, and a rotating cast of aides who each held different fragments of her life story. None of this material consolidates automatically, and funeral homes partnering with multi-site senior living operators face the coordination problem every time a resident in their care network passes.
Research on distributed team processes in healthcare identifies specific coordination barriers that apply directly to multi-site memory care story collection: information asymmetry across sites, different documentation practices, and loss of tacit knowledge when staff rotate (PMC - Distributed Team Processes Healthcare). A mixed-methods analysis of multi-centre qualitative research confirms that diverse-site coordination enables richer participant engagement but requires explicit infrastructure to prevent data fragmentation (PMC - Multi-Centre Qualitative Research Methodology). Funeral homes trying to gather stories from memory care patients who have moved through multiple facilities encounter exactly this fragmentation at the most time-pressured moment of the family relationship.
Weaving Multi-Site Story Threads Into a Coordinated Tapestry
StoryTapestry is designed around the assumption that memory care patients rarely spend their final years in a single facility. The tapestry metaphor is operationally useful here because threads from six different sites (two assisted living communities, a memory care unit, a hospice, a day program, and the family home) weave into a single coherent tribute only when the collection infrastructure actively supports cross-site workflows. The alternative is six separate fragmentary collections that arrive at the funeral home as six folders the director must manually merge.
The structural model borrows from coordinating centers in multisite healthcare research (RTI - Coordinating Centers). StoryTapestry functions as the coordinating center across the senior living network: each facility has site-level access for its own staff and residents, but a designated program coordinator at the funeral home sees the full picture when a resident transfers or dies. Lessons from the CSER consortium on data coordination across sites inform the platform's permission structure (PMC - CSER Data Coordination Lessons): facility-level autonomy for daily collection, centralized harmonization for cross-site assembly, and clear handoff protocols when care transitions occur.
Florence Healthcare's analysis of four common challenges in multicenter research maps directly to memory care story coordination: protocol adherence variations, communication bottlenecks, data quality differences, and site capacity disparities (Florence Healthcare - Multicenter Challenges). The protocol-adherence problem in memory care looks like this: Site A collects detailed life stories during intake, Site B does paper life story books nobody updates, Site C relies on an informal "resident bio" form that sits in an unshared folder. StoryTapestry solves protocol variation by providing a shared intake workflow that facilities can adopt at their own capability level while still contributing to a unified patient record.
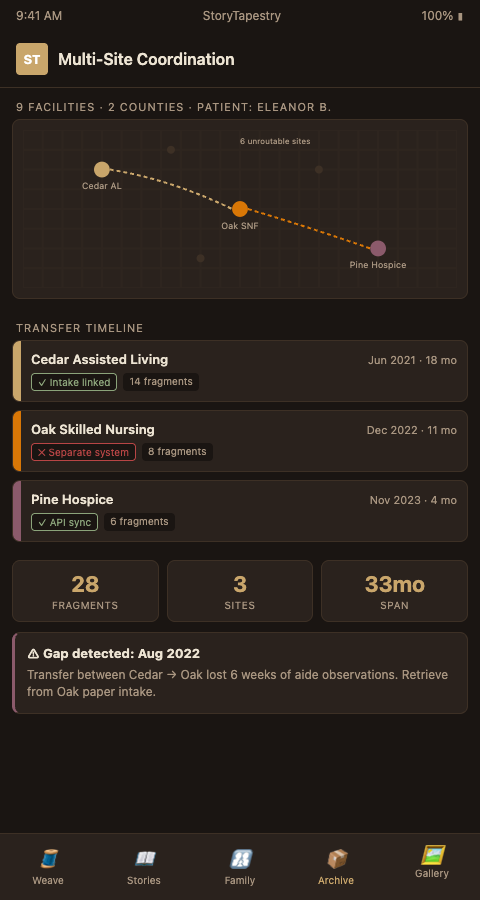
Multicenter trial management systems provide templates for synchronized orchestration across sites (JMIR - Multicenter Trial Management System). StoryTapestry applies similar orchestration logic to bereavement collection. When a patient transfers from a partner assisted living community to a partner memory care unit, the life story follows automatically, with new staff at the receiving facility inheriting the archive rather than starting from zero. This integrates with digital story collection at the site level and connects upward to bereavement program scaling at the network level.
The permission architecture is the load-bearing technical detail that makes multi-site coordination work without creating privacy or liability problems. Each facility's staff see only the residents currently at that site, which matches their clinical need-to-know scope. The funeral home coordinator sees the full cross-site picture for residents whose families have designated the home as their memorial partner, which is the scope that prevents fragmentation at death. Family contributors see only the threads they are authorized to see, which is typically everything about their own loved one and nothing about other residents. This three-tier structure looks simple in documentation but requires careful engineering to hold up across the real-world complexity of transfers, discharges, readmissions, and family structure changes.
StoryTapestry's permission model has been tested against the transfer scenarios memory care networks actually produce and reliably prevents both under-sharing (new site cannot see the archive) and over-sharing (cross-resident exposure) that coordination in spreadsheets cannot achieve.
Advanced Tactics for Multi-Site Story Coordination
Five tactics help memory care funeral homes coordinate effectively across facility networks. First, establish quarterly protocol alignment reviews with facility program coordinators. New staff at each site need onboarding to the shared intake workflow, and site-level practice drifts over time unless reviewed deliberately. A quarterly 45-minute video call that walks through recent coordination successes and gaps keeps protocol adherence above 85% across a 6-to-10 facility network without heroic effort. Without this rhythm, adherence drops below 60% within two quarters, and the coordination value collapses back to informal partnership theater.
Second, handle time zone coordination explicitly when the partner network spans multiple states or when family contributors live across time zones. A California assisted living community transferring a patient to an Arizona skilled nursing facility while the primary caregiver daughter lives in Boston creates a three-time-zone coordination problem that pure local workflows cannot solve. StoryTapestry's asynchronous contribution model lets each contributor work in their own window while maintaining a unified collection timeline that the coordinating center reviews weekly.
Third, build cross-site story audit reports into the monthly partnership review with facility administrators. The report shows which patients at each site have rich story collections, which have thin collections, and which facilities are capturing more versus less material over time. Administrators use this to prioritize staff training and to demonstrate the partnership's value to their boards when budget cycles tighten. Memory care facility chains increasingly select funeral home partners based on measurable contribution to resident life story programs rather than service pricing alone.
Fourth, handle facility contract transitions deliberately. When a memory care chain is acquired, when a single facility changes ownership, or when a funeral home loses a contract with one site in a network, the life story archives for affected residents need an explicit disposition plan. StoryTapestry's contract transition workflow produces a family notification sequence that explains what is changing, a data migration option if the family wants their loved one's archive moved to a new coordinating home, and a preservation option if the family wants the archive retained independently regardless of future business relationships. Without this workflow, contract transitions destroy years of contributor investment and produce legal exposure around data ownership that memory care funeral homes should not accept.
Fifth, establish an incident response protocol for multi-site coordination breakdowns. When a resident dies unexpectedly at one facility while mid-transfer to another, the coordination workflow that was mid-stream is suddenly the critical path to the memorial. StoryTapestry's incident response mode consolidates the fragmentary records from both sites, flags what is missing, and produces a prioritized outreach list for the funeral home to complete collection within the narrow window before the service. Incident mode is used roughly once per 40 deaths across a mature network, which is rare enough that ad-hoc handling is tempting but frequent enough that having a protocol prevents the fragmented memorials that otherwise result.
Build Multi-Site Coordination Infrastructure With StoryTapestry
Funeral homes that serve multi-facility memory care networks without coordination infrastructure will continue to produce fragmented memorials when patients pass after complex care journeys. Those that adopt shared cross-site workflows produce coherent tributes and become preferred partners for regional and national senior living operators. StoryTapestry delivers the coordinating-center architecture, protocol alignment tools, and cross-facility transfer workflows that make multi-site story coordination operational. Reach out to StoryTapestry to scope a partnership model that fits your memory care funeral home's facility network and the families who move through it.
Pilot funeral homes with multi-site senior living networks receive product team support to map their current facility partnerships, design the site-level permission architecture, and establish the quarterly protocol alignment cadence with program coordinators across their network. Your first cross-site memorials on the platform receive concierge support across the full transfer path, which means the product team walks alongside your coordinator when a resident moves from assisted living to memory care to hospice and the archive successfully follows all three transitions. Your feedback shapes the production release of the transfer workflow, the cross-site audit reporting, the contract transition data-portability tools, and the incident response mode that handles coordination emergencies when residents die unexpectedly mid-transfer.
Schedule a consultation to scope a partnership model that fits a regional senior living network of 6-to-10 facilities or a national chain with dozens of sites, and to understand how your funeral home can become the preferred memorial partner those networks select on the basis of measurable life-story continuity rather than service-tier pricing.