How Dementia Hospice Teams Can Coordinate Funeral Home Story Handoffs
The Problem with Ad Hoc Hospice to Funeral Handoffs
Hospice care for dementia patients produces a unique knowledge base: weeks or months of intimate observations by clinical staff who witness moments family often do not see. Yet standard handoffs from hospice to funeral home transfer little beyond death certificates and body transport logistics. According to PMC research on transitions to hospice for dementia, these transitions are shaped by caregiver burden and prognostic uncertainty, with communication gaps consistently documented across the care journey. PMC research on transition-to-hospice perspectives confirms staff describe communication gaps during hospice transitions as a recurring problem.
Structural barriers exist. NCBI research on handoffs' implications for nurses documents that effective handoffs require structured transfer of essential information, but existing tools focus on clinical data, not narrative material. VITAS Healthcare's hospice guidelines for dementia include clinical criteria like FAST scale 7C for eligibility, but nothing about story capture. The result is that the hospice chaplain's notes on a patient's response to music, the aide's observation of his morning ritual, and the social worker's conversation with the estranged daughter all vanish at the transition point.
Weaving a Continuity-of-Care Story Handoff
The framework StoryTapestry proposes is to treat the hospice-to-funeral-home transition as a thread handoff, not a restart. When a dementia patient enters hospice, the funeral home's memorial tapestry opens (if it hasn't already) and the hospice team begins contributing directly. Chaplains, nurses, aides, and social workers each have contributor accounts tuned to their vantage points. Their observations become threads in the tapestry during the active care period, not after it. By the time the patient dies, the funeral home has weeks of texture already woven, and the family meets a memorial in progress rather than a blank page.
Alliance for Care at Home guidance on Medicare hospice bereavement CoP notes Medicare requires hospice bereavement services for up to one year post-death. That regulatory framework aligns perfectly with a tapestry-based handoff because both hospice and funeral home have a shared year-long obligation to the family. Hospice Foundation of America's guide on hospice bereavement compliance formalizes these requirements, and a shared tapestry operationalizes them into one continuous workflow rather than two disconnected programs.
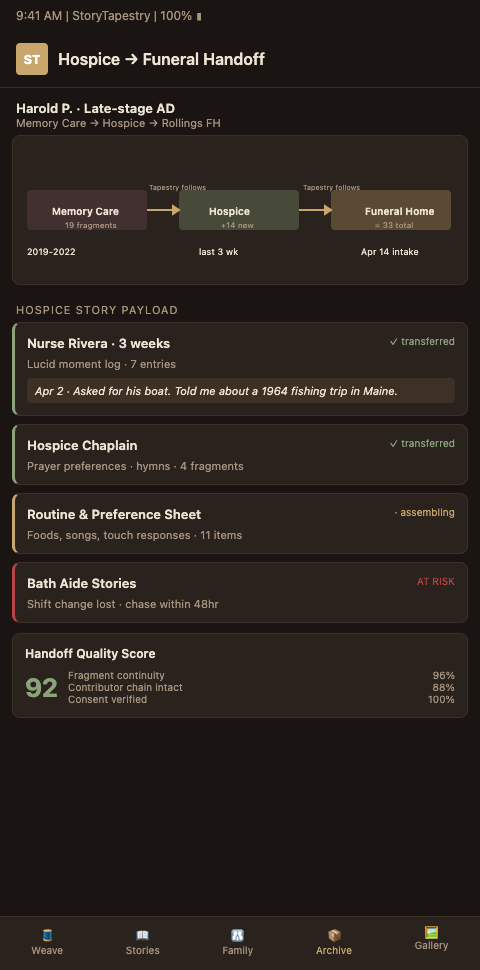
Operationally, the handoff runs on three protocol layers. First, a credential layer: hospice staff contributors sign in via organizational SSO, so permissions travel with employment rather than requiring per-family onboarding. Second, a prompt layer: hospice chaplains see prompts tuned to spiritual and relational observations, while aides see prompts tuned to daily routines and sensory preferences. Third, a privacy layer: family reviewers can approve threads for the public tapestry or keep them in the private archive, which matters especially for hospice chaplain notes that may touch sensitive family dynamics.
Cognitive-Stage Sensitive Prompts are especially important at the hospice stage. Patients in FAST 7 have limited verbal capacity, so prompts to staff focus on non-verbal observation. "What does she respond to?" unlocks threads that "What has she said?" cannot. These prompts connect naturally to funeral home partnerships that span the full care journey rather than starting at the death event.
Pre-Decline Proactive Gathering becomes retroactive at the hospice stage, but the tapestry still weaves early-stage family contributions with late-stage hospice observations into one memorial. When the family sees the completed tapestry, they see the full arc: their loved one at their most present, their loved one in hospice, and the many voices who witnessed both. This connects to multi-site coordination practices that matter when patients move across care settings — home, memory care facility, hospice unit — during their final months.
Contributor workload on hospice staff has to be calibrated carefully. A hospice nurse caring for 10 to 15 patients simultaneously cannot realistically contribute long narrative threads to every patient's tapestry, and asking her to do so produces either burnout or resentment. The sustainable model is short structured contributions (a 30-second voice memo, a two-sentence observation, a single photo with caption) timed to shift handoffs or care conferences already on the clinical calendar. The hospice social worker typically contributes longer threads that synthesize across multiple staff observations, which reduces the frontline staff's individual burden while still capturing their collective witness. Funeral home liaisons who understand hospice staffing realities build contribution protocols that respect the clinical workflow; liaisons who push harder ask patterns damage the partnership and end up with thinner threads than a well-calibrated protocol would produce.
Advanced Tactics for Hospice-Funeral Handoff Integration
The most common mistake is treating the handoff as a technology problem rather than a relationship problem. Funeral homes that sign a data-sharing agreement with a hospice without embedded liaison relationships get little usable material. The handoff works when the hospice social worker knows the funeral home's bereavement lead by name and has a standing biweekly check-in during active cases. The tapestry platform supports the relationship; it does not replace it.
Edge cases worth scripting. Hospice patients who transition between hospice agencies (not uncommon for dementia) need contributor continuity across agencies. Patients who enter hospice from home rather than a facility need family-facilitated onboarding of hospice staff contributors, because there is no facility admin to coordinate credentials. Patients whose death occurs faster than expected (a common reality in late-stage dementia) need rapid-window intake that captures the hospice team's observations even if the full care period was brief.
Training deserves investment. Hospice staff contributing to a memorial tapestry should understand the difference between clinical documentation and narrative contribution. Clinical notes are structured, timestamped, and objective. Memorial threads are personal, observational, and attributed. The same nurse writes different material in each format. A two-hour training during onboarding, refreshed annually, dramatically improves thread quality. Include short video examples of strong and weak threads from actual memorials (anonymized with family permission), because practitioners learn the difference faster from examples than from abstract instruction.
Measure handoff health with three signals: percentage of hospice deaths where at least one hospice staff thread is in the final memorial, average days between hospice admission and first hospice thread, and family ratings of memorial completeness in the year post-service. Firms with rising numbers on all three are operating the handoff correctly.
Regulatory alignment is a strategic advantage when the hospice-funeral partnership is built thoughtfully. Medicare's bereavement CoP requires hospices to provide a year of bereavement services, and funeral homes that share platform infrastructure with hospices can help their partners meet this requirement with less effort than standalone bereavement programs require. The shared tapestry becomes the continuous artifact that serves the hospice's regulatory obligation and the funeral home's family service obligation simultaneously. Hospice agencies increasingly evaluate funeral home partners on whether they extend rather than duplicate the hospice's bereavement work, and a shared platform is the most visible signal that the funeral home has designed the partnership for mutual operational benefit rather than one-sided referral extraction.
Cross-organizational governance prevents partnership drift after the initial enthusiasm fades. A quarterly review meeting with named hospice and funeral home leaders on both sides, a shared metric dashboard that tracks handoff completeness and family outcomes, and a formal protocol refresh every 18 months keeps the partnership operating at design intent rather than drifting into informality. Hospice agencies with multiple funeral home partnerships quickly identify which partners run formal governance and which run on personality. Firms that maintain structure outlast the staff turnover that would otherwise dissolve the relationship. The same governance pattern underpins memorial handoff protocols in perinatal loss care, where hospital teams hold irreplaceable observation that funeral homes need access to through the same kind of durable cross-organizational structure.
Start Coordinating Hospice Story Handoffs for Dementia Families
Memory Care Funeral Homes joining the StoryTapestry waitlist get early access to the hospice-to-funeral-home handoff workflow, including hospice staff contributor onboarding, role-based prompt libraries, and family reviewer routing. If your firm partners with hospice agencies serving dementia patients and has watched irreplaceable hospice team observations vanish at the transition point, this workflow bridges the gap with structure and respect. Reserve a pilot slot to help shape the credential protocols, training modules, and biweekly relationship cadence for your hospice partners.
Pilot partners work with the StoryTapestry product team to design the specific credential integration with their hospice partner's clinical systems, to train hospice staff on the contributor interface, and to establish the governance cadence that sustains the partnership across staff turnover. Your firm's first three hospice-transferred memorials receive concierge assembly support during the 90-day pilot window, which means the protocol is stress-tested on real cases with expert support before your directors operate it independently. Your feedback shapes the production release of the hospice staff onboarding flow, the clinical-to-narrative training modules, and the shared bereavement CoP reporting features that extend the platform's value to your hospice partners. Reserve a pilot slot now to build a hospice handoff capability before your competitors do, because the hospice agencies in your market are actively evaluating funeral home partners on exactly this capability.