5 Ways Funeral Homes Can Partner with Memory Care Facilities
The Problem with Informal Referral Lists
The standard relationship between funeral homes and memory care facilities is a business card exchange and an occasional lunch. When a resident dies, the administrator hands the family a brochure, and the funeral home's first interaction with the deceased is transport day. According to PMC research on transitions to hospice for dementia, care transitions are determined by caregiver burden, prognostic uncertainty, and communication gaps. The same factors shape the eventual memorial, which means funeral homes entering the story only at the end inherit the communication debt that accumulated across the care journey.
Market conditions reward firms that fix this. Allied Market Research on the funeral services market projects steady growth driven by personalization demand and family expectations. The NFDA 2025 consumer study reports Americans embracing digital funeral planning while still seeking professional guidance, which favors funeral homes with structured intake tools over those relying on informal relationships. Funeral homes with deeper memory care partnerships capture the pre-need planning conversation years earlier and arrive at the death with a tapestry already in progress.
Five Partnership Models That Weave Lasting Relationships
Model one is the bereavement program integration. Homesteaders Life on funeral service and hospice partnerships describes how shared common purpose creates meaningful collaboration. Apply that to memory care by embedding a funeral home bereavement liaison into the facility's family support meetings. The liaison does not sell services during these sessions. They listen, take notes on family dynamics, and capture early story fragments for the resident's eventual memorial tapestry.
Model two is the pre-decline story gathering protocol. When a resident progresses to moderate-stage dementia, the facility triggers a StoryTapestry intake session during the next care-plan meeting. Families contribute what they can. Staff add their observations. The tapestry grows quietly in the background for months or years. This aligns with Alzheimer's Association hospice care guidance, which emphasizes preparing families for end-of-life transitions well before the final weeks.
Model three is the staff contribution partnership. Memory care CNAs and activity staff know residents in ways family cannot, especially in later stages. Formalize their contribution by carving out 15-minute story sessions during shift handoffs, routed through StoryTapestry's caregiver fragment collection flow. This produces the kind of staff memorial contributions that transform a memorial from generic to specific.
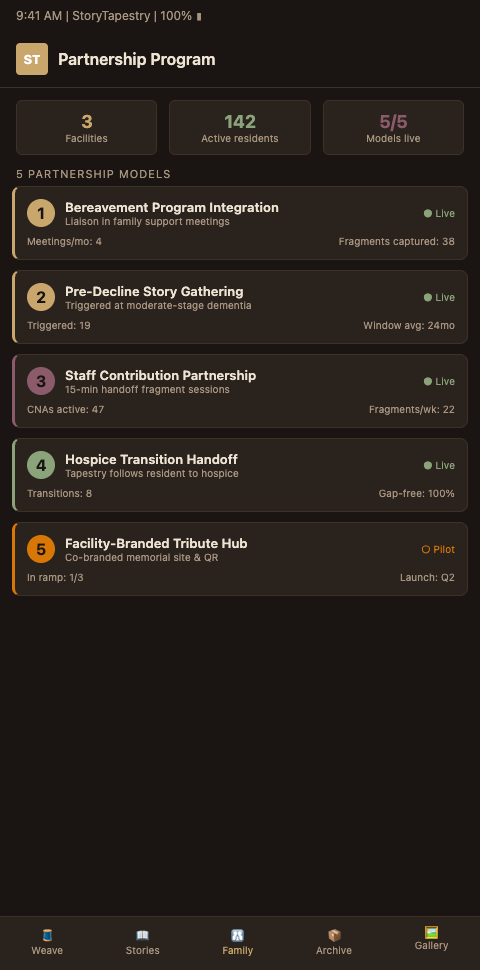
Model four is the hospice transition handoff. When a memory care resident enters hospice, the story already in progress transfers with them. The funeral home's tapestry continues gathering threads without restart. This avoids the gap hospice story handoffs typically fail to bridge, where each care setting collects different fragments and none share.
Model five is aftercare continuity. Johnson Consulting on elevating funeral home aftercare makes the case that aftercare programs drive lasting community impact. For memory care families, the aftercare becomes a year of tapestry refinement. Families can add newly surfaced photos, stories from distant relatives who attended the service, and sibling reconciliation threads that only emerged during grief. The memorial tapestry stays living, which is both a service to the family and a retention lever for pre-need conversations with their own eventual planning.
The core metaphor runs through all five models. Each partnership weaves a different kind of thread into the same permanent tapestry. Pre-decline gathering contributes the biographical arc. Staff contributions add sensory and routine detail. Hospice transfer fills the final-months texture. Family sessions during active grief add the relational layer. Aftercare fills gaps that only become visible after the acute grief lifts. StoryTapestry holds all five streams in one memorial, preventing the fragmentation that informal partnerships produce.
Contract structure separates durable partnerships from ceremonial ones. A signed MOU that defines each side's commitments (facility provides staff time and family introductions; funeral home provides training, platform access, and aftercare support) creates accountability that brochure-exchange relationships lack. The MOU should include quarterly review checkpoints, defined staff liaisons on each side, and clear exit provisions so neither party feels trapped. Funeral homes that skip the contract stage typically see the relationship drift within 18 months as staff turnover erodes the informal understanding that made it work in the first place. A two-page MOU is the cheapest possible insurance against that drift and signals to facility administrators that the funeral home is serious about the partnership rather than shopping for referrals.
Advanced Tactics for Partnership Rollouts
Start with one memory care facility per director, not three. Directors need time to learn each facility's care-plan rhythm, which staff hold the longest resident relationships, and which families respond to which contact cadence. Funeral homes that sign MOUs with five facilities in a quarter typically find two become real partnerships and three stall at the brochure-exchange stage. The fix is a 90-day pilot per facility with named staff liaisons on both sides.
Edge cases worth scripting: residents whose families are estranged, residents whose primary caregivers are non-family paid companions, and residents with no surviving family at all. Each needs a distinct intake branch. Paid companions often hold the richest story fragments but lack legal standing to authorize memorial publication. The tapestry should capture their threads but route publication decisions through the facility's ombudsman or a family mediation step.
The common mistake is treating the memory care partnership as a referral pipeline first and a bereavement program second. Firms that lead with referral volume burn trust quickly. Firms that lead with genuine family support find the referrals follow. The same principle applies in the related pattern of military digital memorials, where funeral homes serving veterans find pre-service story gathering builds the relational foundation for later business.
The other mistake is assigning partnership work to the most junior director in the firm. Memory care administrators are senior operators who have spent years managing family expectations, staff turnover, and regulatory scrutiny. They recognize within minutes whether the funeral home has sent a serious counterpart or a bag carrier. Assign a director with five or more years of experience and clear authority to commit the firm, and the first meeting moves from exploratory to operational quickly. Junior directors can shadow the relationship and gradually take over as the partnership matures, but the senior presence at the start defines how the facility rates the funeral home for the next decade.
Measure partnership health with three signals: number of stories gathered before death per resident, percentage of families using aftercare tapestry editing in the year following, and staff contribution rate across shifts. Facilities with rising numbers on all three signals become long-term partners. Those with flat staff contribution rates need operational intervention before any referral volume is possible.
Partnership economics deserve honest accounting. The investment in staff training, platform setup, liaison meetings, and MOU drafting is real, and the payoff comes over 18 to 36 months as pre-need conversations mature and families refer other families from the same facility network. Funeral homes expecting quarterly referral lifts will disappoint themselves and their facility partners. Firms that model partnership as a three-year compounding investment see the math work out: a single facility producing two memorial families per quarter who each refer two more families within 18 months generates substantial book-of-business growth, but only if the initial partnership years are underwritten as relationship infrastructure rather than a referral funnel.
Rollout sequencing matters when a funeral home is signing multiple facilities. Stagger the launches so directors can focus on one new partnership per month for the first four months, then reassess. Parallel launches across four facilities in a single month overwhelm the director team, fragment training attention, and produce mediocre partnerships at all four sites rather than strong partnerships at one. The discipline of sequential rollout feels slower to leadership pressing for portfolio growth but produces faster eventual volume because each strong partnership becomes a reference the funeral home can cite when approaching the next facility.
Start Memory Care Partnerships That Serve Families First
Memory Care Funeral Homes joining the StoryTapestry waitlist get early access to the five-model partnership playbook and the intake workflows that power each stage. If your firm partners with Alzheimer's and dementia facilities but struggles to move beyond the informal referral list, the platform gives your directors structure for pre-decline gathering, staff contribution sessions, and aftercare continuity in one memorial tapestry. Reserve a pilot slot to help shape how the system handles facility MOUs, liaison training, and the cadence of cross-organizational story sessions in your local market.
Waitlist partners get direct access to the partnership playbook, the MOU templates we have tested with early facility partners, and the quarterly review structure that keeps relationships durable across staff turnover. Your directors and facility liaisons receive supervised onboarding during the first 90 days, so the switch from informal referral to structured partnership happens with product-team support rather than trial and error. As an early partner, your firm also contributes feedback on the training modules, the staff contribution interfaces, and the aftercare cadence, which means the production release of StoryTapestry reflects the realities of how funeral homes and memory care facilities actually work together in your region. Reserve a pilot slot now to build the foundation for memory care partnerships that compound across the coming decade rather than relationships that stall at the brochure-exchange stage.