Best Practices for Hospital-Funeral Home Memorial Handoff Protocols
The Problem: Continuity That Breaks at the Hospital Door
The Sands UK charity, now in its fifth decade of working with stillbirth and neonatal loss, reports that the sharpest drop in families' sense of being cared for happens at hospital discharge. The bereavement photographer has come and gone, the memory box is packed, and the parents cross a parking lot with a bag. A week later they are sitting with a funeral director who has none of the context the hospital team had. An analysis in PMC on desired care after discharge found that mothers consistently name continuity of care as their top unmet need after infant loss.
International pathways like the UK NBCP Stillbirth Pathway standardize what hospital bereavement should look like inside the hospital, but the handoff out of the hospital remains uneven. A PubMed review of NICU bereavement care follow-up concluded that mutual healing between clinical and funeral teams depends on shared tools, not on repeated retelling by the family. A PubMed analysis of perinatal clinical practice guidelines found that international consensus on post-perinatal bereavement care does not exist — each region is writing its own playbook, and most of them stop at the hospital door.
The family ends up as the handoff mechanism. They carry the memory box, they retell the medical story to the funeral director, they explain who was in the delivery room, they re-describe what the baby looked like. Every retelling costs. A protocol that removes the family from the handoff is not a convenience — it is a bereavement intervention.
Solution Framework: A Weave That Crosses the Hospital Boundary
StoryTapestry treats the hospital-to-funeral-home transition as one continuous weave. The hospital lays the first threads; the funeral home adds the next row. The family walks through without having to carry the loom.
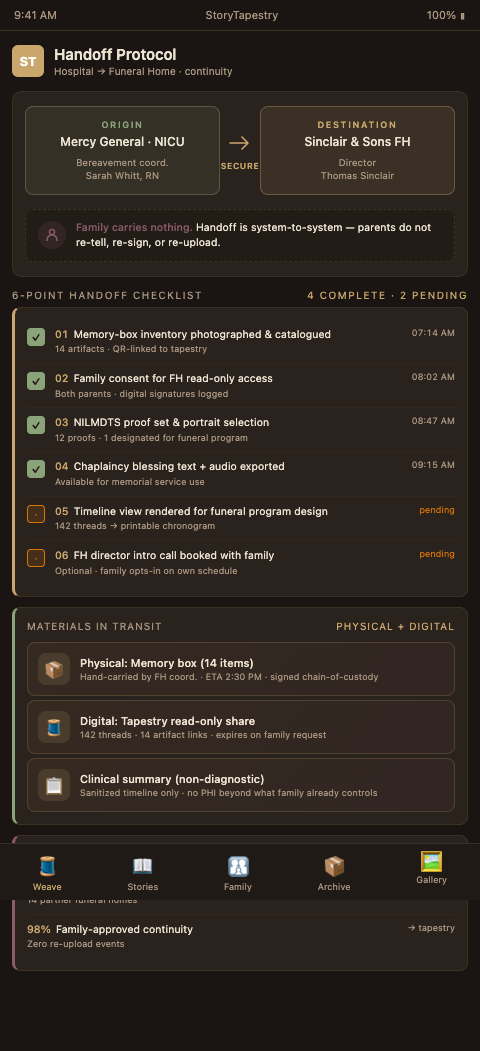
The first element is a handoff packet with two components: a human-readable memorial summary and a structured data export. The human-readable summary is a one-page document naming the baby, the key dates, the preferred pronouns, the names the family uses for siblings and grandparents, and any rituals already performed (blessing, baptism, photography session). It is written for a funeral director reading at 7am before a family meeting. The structured export is a digital artifact: the StoryTapestry tapestry-in-progress with whatever threads the hospital captured, shareable via a time-limited link the family controls.
The second element is consented identity. The family nominates the receiving funeral home during the hospital stay or at discharge. StoryTapestry generates a signed access grant that the funeral home can redeem to become an authorized contributor to the tapestry — not a viewer, but a weaver, able to add threads representing the graveside service, the urn photography, the final resting place. When the family arrives at the funeral home, the director already sees the hospital-laid threads. No retelling required.
The third element is a receiving protocol on the funeral-home side, modeled on programs like CHOP's perinatal palliative care and bereavement coordination. The funeral home's intake meeting uses the hospital-provided summary as its agenda rather than an intake form. The director asks clarifying questions — "the summary notes you called her Poppy, is that what you'd like engraved?" — instead of discovery questions. Meetings shrink from 90 minutes to 40, and the family leaves the first meeting with a draft order of service built on what the hospital already documented.
The fourth element is bidirectional. When the funeral home adds service photography, floral arrangements, and the memorial card, those threads return to the tapestry and become visible to the hospital bereavement teams who cared for the family. This closes the loop the PubMed NICU follow-up review identified: nurses who cared for a baby who died often never learn what happened after discharge, and that information gap contributes to compassion fatigue. A shared tapestry gives the clinical team a way to witness the service without attending.
The fifth element is durability. The tapestry outlives both the hospital episode and the funeral service. Access permissions shift over time — the funeral home's write access expires 90 days after services conclude, the hospital's expires at discharge, and the family retains permanent ownership. This matches ACOG and ISA international stillbirth alliance recommendations on long-term bereavement support that transcends any single institution.
Tight OB unit coordination is the hospital-side precondition for this handoff to work. A unit that cannot coordinate across L&D, postpartum, and pastoral care cannot coordinate across the hospital boundary to a funeral home. Solve the internal coordination first, then extend outward.
The five elements compound. Without the handoff packet, the funeral director has nothing to work from. Without consented identity, the packet is a document with no address. Without a receiving protocol, the document is handed to a funeral home that does not know what to do with it. Without bidirectionality, the clinical team never learns what the family needed after discharge, and the handoff remains one-way. Without durability, the tapestry expires when the last institutional contract ends. A program that implements only the first three elements produces a better handoff than the status quo but loses the feedback loop that makes the program improve over time. The fourth and fifth elements are not optional features; they are what turn a protocol into a practice.
One practical implementation note: the access grants should be signed during the hospital stay, not at discharge. A mother signing a funeral home nomination form while still on the postpartum unit is clearer, calmer, and more legally sound than a mother signing the same form in a discharge packet she skims on the way out. L&D nurses often resist this timing because it feels intrusive to ask about funeral homes at the bedside. The fix is scripting: "We have partnered with three funeral homes that specialize in babies. If you know which one you would like, we can let them know today so they are ready for you. If you are not ready to choose, we will keep this open for you." The script works because it positions the conversation as service delivery rather than urgency.
Advanced Tactics for Robust Cross-Institutional Handoffs
Four practices strengthen the handoff beyond the baseline protocol.
First, establish named partner funeral homes. A hospital program that partners with 3-5 local funeral homes in its catchment area — training their staff on the StoryTapestry receiving workflow, exchanging on-call contacts, running joint case reviews quarterly — produces faster, smoother handoffs than an ad-hoc model where every loss goes to a different funeral home. Similar bilateral arrangements between funeral home military honors specialists and VA facilities show the same pattern: institutional partnerships outperform one-off coordination.
Second, build a fallback for out-of-network funeral homes. When a family chooses a funeral home the hospital has never worked with, the protocol should still work. StoryTapestry provides a self-service funeral-director onboarding flow — a 15-minute walkthrough that grants write access, explains the thread taxonomy, and provides a starter template for the service-day threads. Hospital staff do not need to be in the loop.
Third, track handoff completeness as a quality metric. A hospital bereavement program can measure the percentage of discharged families whose memorial packet was successfully received by a funeral home within 72 hours, and the percentage of funeral-home-returned threads that flow back to the hospital. Both metrics correlate with family-reported satisfaction at 6-month follow-up. Units that do not measure this tend to assume the handoff is working when it is failing silently.
Fourth, preserve a family-absence workflow. Some families do not have the capacity to nominate a funeral home in the hospital; some have no funeral at all. The protocol should gracefully degrade — the tapestry persists without a funeral-home extension, and a hospital-only memorial is fully coherent. Never design the protocol in a way that makes non-funeral paths feel like failure.
Finally, audit the handoff narrative script. Staff handing a packet to a family should use language that does not imply obligation: "this is yours to share with whoever comes next, or to keep" beats "please give this to your funeral director." The first respects autonomy; the second manufactures a chore.
Build a funeral-home reverse orientation. Most partner funeral homes have never toured the bereavement unit at the hospital that refers to them. Running a quarterly two-hour orientation for funeral directors inside the L&D and NICU units — with the bereavement coordinator walking them through the memory box protocol, the typical family timeline, and the emotional geography of the unit — transforms how the funeral home receives families. A director who has stood in the room where a mother held her son for the last time asks different questions three days later at the funeral home than one who has only read about it. Programs that invest in reverse orientation report that handoff quality improves within the first quarter.
Create a shared case-review cadence with partner funeral homes. Every quarter, the hospital bereavement coordinator and the lead director at each partner meet for ninety minutes to review cases. The review is a joint retrospective where both sides name what worked, what broke, and what the family signaled through the two-week post-service feedback form. Programs that do this find that the second year of partnership produces markedly better handoffs, because the review surfaces small friction points — a consent form the funeral home had to re-collect, an access grant that expired before services finalized, a clinical detail missing from the summary — and corrects them between cycles.
Design the protocol for bilingual families. Hospitals serving Spanish, Mandarin, Vietnamese, or other non-English-primary families need handoff summaries in the family's preferred language, funeral partners who serve those communities, and coordinator capacity to hold consent conversations without a racing telephone interpreter. StoryTapestry supports multilingual summaries that preserve tapestry thread content in the original language of contribution. A grandmother's Vietnamese blessing remains in Vietnamese on the funeral director's copy; a translation appears only if the family requests it.
Document the after-service thread flow explicitly. Many funeral homes complete the service and then go silent on the tapestry. The protocol should specify which threads the funeral home is expected to contribute (order of service, photography, eulogy text, graveside photograph) and by what date, typically two weeks. A coordinator noticing a partner consistently missing the deadline can address it in quarterly review rather than months later when a family asks where the photos are.
CTA: For Hospital Bereavement Programs Formalizing Funeral-Home Handoffs
Your best nurses are already doing some version of this handoff, often from memory and personal commitment, and the inconsistency shows up in post-discharge family surveys. StoryTapestry turns the handoff into a shared protocol with signed access grants, bidirectional thread flow, and a funeral-home onboarding path that does not require your staff.
Invite your bereavement coordinator and two partner funeral directors to a joint 60-minute walkthrough. We'll model the protocol on a recent case — de-identified and drawn from your own unit — and show both sides of the handoff in the same session, from the bedside consent conversation through the two-week post-service feedback review. Seeing the hospital side and the funeral home side in the same room, with the same case, accelerates the work of aligning on protocol more than any written document.
Most programs pilot the handoff with two or three partner funeral homes and expand once the first year's cases demonstrate measurable improvement in family-reported continuity. The pilot produces a handoff protocol document, a consent template reviewed by both your compliance office and the funeral home's operations manager, a training curriculum for new L&D staff, and a quarterly case-review cadence that keeps the protocol tuned to reality. We do not ask your team to invent any of this from scratch; we bring templates from working programs and adapt them to your unit's patient population, staffing model, and funeral home network.