Capturing Profound Moments: Story Fragments from Brief Lives
The Problem: Profound Moments That Slip Away Before Anyone Writes Them Down
The NICU attending physician remembers the way the baby's fingers closed around the father's thumb before the ventilator was removed. The nurse remembers the exact second the father began singing. The lactation consultant remembers the mother asking if she could still pump — just for one day, just to say she had. None of these moments will appear in the medical record. None will appear in the obituary. And unless someone asks, none will appear anywhere the family can revisit them.
Perinatal loss care has advanced substantially in the last decade. A scoping review of memory-making practices published in peer-reviewed literature identified memory-making as a central theme in parents' perceptions of neonatal end-of-life care — yet the review also documented persistent gaps in how those memories are captured, preserved, and made retrievable after discharge. Narrative inquiry research in NICU settings found that parents' stories about their babies contain dimensions the clinical record cannot capture — the textures, the scents, the sounds, the moments of recognition between parent and child. A 2025 MDPI analysis of perinatal loss trauma concluded that parents benefit measurably from narrative approaches, but only when those approaches are offered with structured support.
The capture problem is not that families refuse to tell their stories. It is that grief rarely produces fluent narrative on demand. Bereaved parents need prompts that respect trauma, permission to skip, and infrastructure that preserves half-started sentences as carefully as finished paragraphs.
The Solution: A Loom for Profound Moments
StoryTapestry treats each profound moment as a single colored thread in a larger weaving. The tapestry metaphor is deliberate: no one thread carries the full story, but every thread matters, and the pattern emerges only when the full cloth is viewed together. Hospital bereavement teams and their affiliated funeral partners use StoryTapestry to capture moments across four specific pathways, each designed to lower the barrier between a remembered instant and a preserved narrative.
Moment-by-moment parent prompts. Rather than asking "tell us about your baby," which overwhelms, StoryTapestry asks thirty small questions spread across thirty days — a structure that also underpins our work on pregnancy loss storytelling depth. What did her hair smell like. What was the first thing you noticed about her hands. What song was playing when you drove to the hospital. Therapeutic writing research with grieving mothers shows that assigning meanings through specific, structured writing reduces the intensity of grief pain over time. StoryTapestry borrows this principle and adapts it for memorial construction — each answer becomes a thread, and the thread weaves into the larger tapestry whether the parent wrote three sentences or thirty.
Medical team contribution channels. The NICU nurse who noticed the baby turned toward her mother's voice. The respiratory therapist who adjusted the ventilator settings to minimize the baby's discomfort. The chaplain who wrote down the words of the blessing. StoryTapestry provides a consent-controlled channel where medical staff can add their own observations, always reviewed by the family before appearing in the memorial. Digital storytelling feasibility research with bereaved families confirmed that multi-voice contribution enriches legacy work without overwhelming primary grievers.
Audio and visual fragment capture. Not every moment fits into text. StoryTapestry accepts short voice memos, ambient sound recordings (the heartbeat monitor, the lullaby the grandmother sang, the father's voice reading the chosen name aloud), and photographs organized by moment rather than by date. The MISS Foundation and similar organizations have long advocated for multi-sensory memory preservation, and StoryTapestry makes the workflow light enough that a nurse can help a family capture three recordings in under ten minutes.
Staged partner and family timelines. Partners often experience the same loss from different emotional positions. Fathers, co-parents, and non-gestational parents report that their grief is frequently overlooked — research on fathers' and partners' bereavement experiences identifies five themes that specifically sustain parental identity across both parents. StoryTapestry preserves parallel voices: two partners can each respond to the same prompt and both answers appear side-by-side in the tapestry, rather than being flattened into a single "parents' voice."
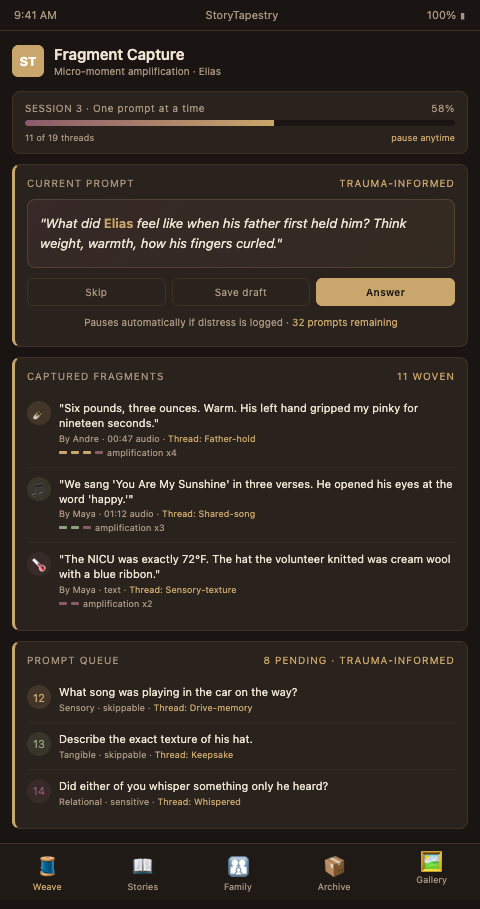
Advanced Tactics for Capturing Profound Moments
The rule of specific detail. Generic memorial language ("she was loved") tells us nothing we did not already know. StoryTapestry's prompts train hospital bereavement coordinators to ask for the smallest possible specific — the shape of the birthmark, the color of the hat, the precise sentence the chaplain spoke. Specific details create tapestry threads with visible texture; generic language fades into background color.
Pause-and-return architecture. A bereaved mother may begin answering a prompt at 2 AM, close the browser after three words, and return six weeks later. StoryTapestry preserves the partial sentence exactly as she left it, never forces completion, and gently reminds her the fragment is there whenever she wants to finish — an approach developed in tandem with our sensitivity collection practices for infant loss programs. This architecture draws from the same evidence base that supports scoping reviews on pregnancy storytelling interventions, which identified pacing autonomy as critical for bereaved engagement.
Verification of contested details. When two family members remember a moment differently — the mother remembers the song as "You Are My Sunshine," the father remembers it as "Brahms' Lullaby" — StoryTapestry preserves both, clearly labeled, rather than forcing a resolution. The tapestry metaphor holds: two threads of different color sit beside each other and the full fabric is richer for it. This approach parallels the rigor needed in cross-generational memorial verification work we support in other niches.
Export-ready memorial artifacts. The tapestry is digital, but families often want printed programs, shadow boxes, or photo books. StoryTapestry exports any subset of the memorial into print-ready layouts that affiliated funeral homes can fulfill. A four-page printed booklet becomes a tangible extension of the online tapestry without duplicating the grieving family's work.
Medical team wellbeing integration. Staff who care for brief lives carry secondary grief, and the same reflection discipline we use for deployment chapter reconstruction with veteran families translates directly to perinatal staff support. When hospital bereavement programs use StoryTapestry, the same platform that holds the family's tapestry also serves as a structured reflection space for the medical team — a place to acknowledge what they witnessed, within the boundaries the family has consented to. This dual function reduces moral injury among NICU staff without breaching family privacy.
For Hospital Bereavement Teams Ready to Capture What Would Otherwise Disappear
Brief lives leave behind profound moments that will vanish unless someone builds the infrastructure to catch them. StoryTapestry was designed with perinatal bereavement coordinators, NICU nurses, and affiliated funeral directors who already do this work — and who have been limited by tools not built for their context. If your hospital bereavement program is ready to extend its documentation beyond the memory box, our team can walk you through a pilot that integrates with your existing consent practices and EHR. The same storytelling infrastructure that honors a four-hour life also supports pregnancy loss narratives of any gestational age, with sensitivity collection guidelines tailored to each clinical pathway, and translates naturally to adjacent bereavement contexts including our deployment chapter piecing work with veteran families. Reach out to schedule a trauma-informed consultation with your unit leadership.