Why Pregnancy Loss Memorials Deserve Full Narrative Depth
The Problem: Pregnancy Loss Grief Rendered Invisible by Systems Built for Other Losses
A woman who miscarried at 14 weeks described the aftermath this way: "I had been telling coworkers I was pregnant for three weeks. Then one Monday I wasn't pregnant, and there was no obituary, no funeral, no time off policy, nothing. People kept saying at least I could try again, like I had lost a phone." Her pregnancy loss generated an ultrasound image, a discharge summary from the emergency department, and a bill from the lab. There was no structure for her grief because the systems around her did not recognize her grief as grief.
Pregnancy loss sits in what researchers describe as disenfranchised grief — loss not socially acknowledged or openly mourned. The APA's reporting on hidden grief of miscarriage documents that miscarriage grief is systematically minimized, leaving bereaved parents without social scripts for mourning. A vignette study on pregnancy loss disenfranchisement confirmed that social disregard elevates psychological burden for grieving parents. Further research on perinatal loss ambiguity traced how ambiguity around viability — the very uncertainty about when a pregnancy "counts" — contributes directly to the disenfranchisement.
The psychological cost is measurable. A meta-analysis of mental health impact after perinatal loss documented elevated depressive and anxiety risk across all gestational ages. A separate study on depression and PTSD found bereaved women had 4x the odds of depression and 7x the odds of PTSD versus non-bereaved controls. Despite these measurable harms, miscarriage and early pregnancy loss remain under-served by memorial infrastructure.
The Solution: Full-Depth Narrative Weaving for Pregnancy Loss
StoryTapestry approaches pregnancy loss with the same structural seriousness it brings to term stillbirth and neonatal loss. The tapestry metaphor holds because it insists that brief lives accrue narrative weight through the accumulation of specific threads — not through a single obituary paragraph. Pregnancy loss memorials built on StoryTapestry acknowledge that the parents' relationship with this baby began at conception (or earlier, at hope and intention) and continues after discharge.
Narrative depth across four pregnancy chapters. StoryTapestry organizes pregnancy loss memorials around four structural chapters: anticipation (before pregnancy), early pregnancy (weeks 1-12), mid-pregnancy (weeks 13-23), and late pregnancy or neonatal (weeks 24+). Each chapter contains its own prompt library tuned to what parents typically remember and want to preserve at that gestational age. This structure draws on Neimeyer's meaning-making research in bereavement, which has established meaning reconstruction as central to grief adaptation. Each chapter is a tapestry panel, and each answered prompt is a thread.
Recognition of partners' and fathers' parallel grief. Research on men's grief following pregnancy loss describes fathers and non-gestational partners as experiencing double-disenfranchised grief — loss minimized by society and further minimized within their own families. StoryTapestry preserves parallel voices: partners can each respond to the same prompt separately, with both answers appearing as adjacent threads in the tapestry rather than collapsed into a single "parents' perspective." This mirrors the cultural storytelling traditions approach we take across different bereavement contexts.
Specific-detail prompting for pregnancy-specific memories. Pregnancy contains memories no one outside the pregnant body holds: the first kick, the specific food aversions, the sensation of the baby's hiccups, the song that always seemed to calm her — the same brief-life moment capture discipline we apply to term losses. StoryTapestry's prompt library asks for these specific details gently and one at a time. A mother who cannot write a eulogy can usually answer "what was the song that always calmed her?" — and that single thread becomes permanent.
Ultrasound and imaging integration. Ultrasound images are often the only photographs of a pregnancy loss. StoryTapestry provides a sensitive ultrasound integration that preserves images with timestamp metadata, gestational age, and parental annotations. The ultrasound is not a medical record in this context — it is a portrait, and the platform treats it accordingly. Families can add the sentences they remember saying when they first saw the image, the question they asked the sonographer, the name they started using afterward.
Sibling inclusion appropriate to gestational age. Older siblings often have a different relationship with pregnancy loss than with neonatal loss — the baby was imagined but never seen. StoryTapestry's sibling module for pregnancy loss includes age-appropriate prompts about the baby they were going to meet, what the child imagined the baby's voice would sound like, what they would have said. These sibling threads become permanent parts of the tapestry rather than conversations that fade.
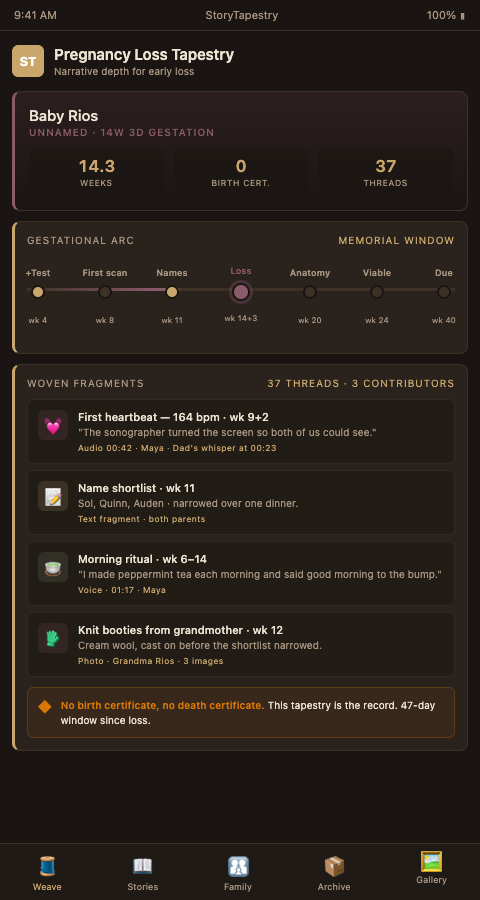
Advanced Tactics for Pregnancy Loss Memorial Depth
Retroactive chapter population after later losses. A family whose first pregnancy ends at 8 weeks may have few artifacts. But if that family later experiences a 20-week loss, StoryTapestry allows the earlier loss tapestry to be revisited and retroactively populated as the parents' narrative capacity grows. Grief develops language over time, and the platform accommodates this developmental reality.
Clinical language translation. Hospital discharge paperwork uses terms like "missed abortion" and "incomplete abortion" that many bereaved parents find painful. StoryTapestry never displays clinical terminology in the family-facing tapestry. When clinical records integrate (with consent), the platform translates medical language into narrative-appropriate phrasing — preserving accuracy while honoring the parents' language and protecting perinatal grief artifact preservation from retraumatizing medical vocabulary.
Anniversary date architecture. Pregnancy loss anniversaries are multiple and complex: the date of loss, the date the pregnancy was confirmed, the would-have-been due date, the date of discharge. StoryTapestry lets families mark whichever dates matter to them and receive gentle, skippable prompts on each. Research on brief-life artifact preservation confirms that multiple anniversary markers reduce the isolation of single-date grief.
Integration with hospital-affiliated funeral services. Many parents do not realize that affiliated funeral homes offer services for pregnancy loss at any gestational age. StoryTapestry includes a clear, non-pressuring pathway for families who want to explore affiliated funeral memorial services — including small keepsake ceremonies, scattered ashes gatherings, or printed memorial artifacts drawn directly from tapestry content.
Community tapestry views. With explicit family consent, hospital bereavement programs can create aggregated, anonymized community tapestry views that show pregnancy loss families they are not alone, honoring the cultural storytelling customs each community brings to the platform. These views preserve privacy rigorously — no names, no photos, no identifying detail — but allow a grieving parent to see the scale of shared loss and the range of how other families have chosen to remember.
Obstetric team reflection thread. Obstetricians, midwives, and L&D nurses who attend pregnancy losses carry their own weight. StoryTapestry's clinician reflection space lets the medical team document — privately from the family — what they witnessed and what they want to remember about the family they cared for. This reduces moral injury without breaching confidentiality.
For Hospital Bereavement Programs Ready to Honor Pregnancy Loss With Full Depth
Your hospital bereavement program may already excel at stillbirth and neonatal loss care. Pregnancy loss — especially early loss — is often the gap. StoryTapestry closes that gap with narrative infrastructure built specifically for the disenfranchised grief of miscarriage, ectopic loss, and early pregnancy loss. We partner with perinatal bereavement coordinators, affiliated funeral directors, and obstetric team leaders to pilot the platform in the units where it will matter most. The same tapestry infrastructure that captures brief life story capture for term losses also preserves perinatal grief artifacts across gestational ages. Reach out to discuss how your program can extend pregnancy loss memorial depth with trauma-informed digital infrastructure.
The initial consultation runs 45 minutes and covers your unit's current pregnancy loss pathway, the gestational-age coverage gaps we see most often in hospital programs, sample tapestries at four-week, 12-week, and 24-week gestational stages, and the disenfranchised-grief prompt library built with perinatal loss families. Pilot engagements include platform access for your bereavement coordinator and one OB nurse lead, a training block for your L&D and emergency department triage teams, and a named implementation lead who supports the first 10 pregnancy loss cases. Most programs onboard their first family inside four weeks and reach protocol-level adoption across all gestational ages by month four. Bring your OB nurse manager, bereavement coordinator, and one emergency department lead — the consultation produces a pathway diagram all three can use with medical leadership.