How to Gather NICU Stories from Medical Staff for Infant Memorials
The Problem: NICU Staff Witness Irreplaceable Moments That the Family Never Hears About
A primary NICU nurse described caring for a baby over six 12-hour shifts across four days. She noticed the baby's preferred sleeping position, the song that seemed to slow the heart rate monitor, the specific way the baby's fingers curled around a swaddle edge. At the end of the fourth day, the family chose compassionate extubation. The nurse was present. She remembered every detail of those six shifts. Three weeks after discharge, when the social worker asked her to write a condolence letter to the family, she found herself unable to fit any of what she had witnessed into a one-page letter.
This gap between staff observation and family memorial is well-documented. Narrative inquiry research exploring parents' NICU stories identified care team reflections as an underused source of memorial material. A qualitative study of end-of-life experiences among NICU providers established that providers actively build relationships and create memories — but documented little infrastructure for sharing those memories with families in structured ways. A Brown University analysis of bereavement debriefing captured how NICU staff themes emerge through structured debriefing, and research on NICU bereavement care follow-up found that families find meaning through keepsake memories shared by medical staff — with benefits for both the family and the healing of the care team.
A phenomenological study of parents' lived NICU experience further confirmed that parents value medical staff support during grief but often cannot recall specific moments staff may have witnessed. Staff memory complements family memory; neither alone is sufficient. Research on parental needs at end-of-life in NICU emphasized the specific benefit of a dedicated bereavement nurse present throughout. Legacy intervention studies confirmed NICU parents' willingness to engage with legacy storytelling when the infrastructure supports them.
Without structured capture, staff observations vanish. Shift change erases them. EHR templates cannot hold them. Condolence cards cannot contain them.
The Solution: A Consent-Controlled Weaving Channel for NICU Staff Contributions
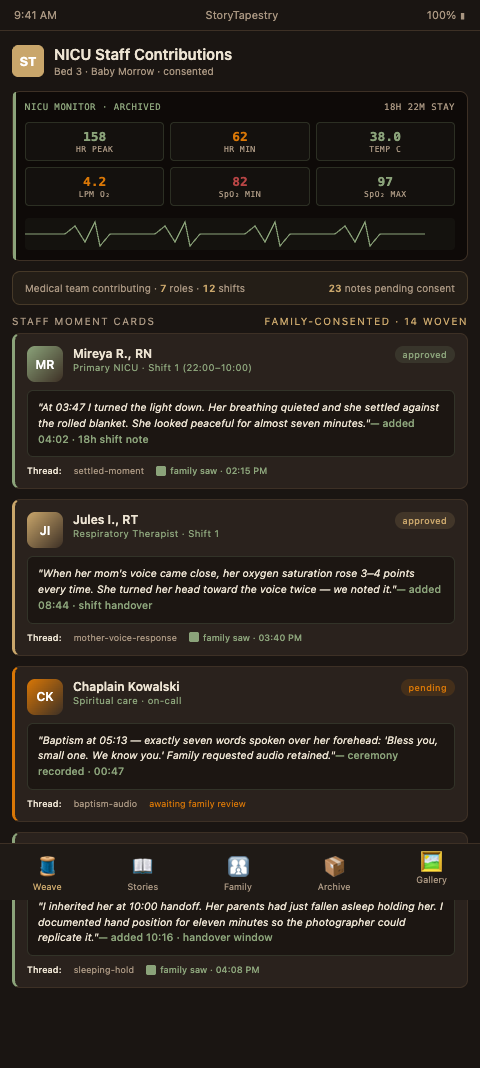
StoryTapestry provides NICU teams a consent-controlled contribution channel that captures staff observations during and after each shift. The tapestry metaphor holds: nurses, respiratory therapists, social workers, chaplains, and attendings each weave their own observation threads, which the family reviews and chooses to include or set aside. The result is a memorial with the density of lived observation rather than the thinness of a single family perspective.
Shift-bound contribution windows. A NICU shift is 12 hours. StoryTapestry provides a shift-end reflection window — three to five prompts that take under ten minutes — where the outgoing nurse can document observations that will not fit in the clinical handoff, anchored in the broader hospital bereavement workflow the coordinator already runs. The prompts are specific: what did the baby seem to prefer, what did you observe about the parents' interaction, what moment surprised you, what would you want the family to know. These reflections are staged and never appear in the family tapestry until the family explicitly accepts them.
Multi-disciplinary observation channels. NICU care involves a team: nursing, respiratory therapy, neonatology, social work, chaplaincy, lactation consulting, child life specialists. StoryTapestry provides role-specific prompt libraries calibrated to each discipline's typical observations. A respiratory therapist is asked different questions than a chaplain, because they witness different dimensions of the baby's life. This mirrors the hospital bereavement teams structure we recommend across contexts.
Family-gated approval workflow. No staff contribution appears in the public tapestry without the family's explicit approval. StoryTapestry displays pending contributions to the family in a gentle, pressure-free interface: they can accept, decline, or request edits. Declined contributions are preserved privately for the staff's own reflection without ever entering the family's memorial. This consent architecture addresses the concerns raised in best-practice bereavement care scoping reviews about clinician voice in family memorials.
Staff wellbeing integration. Secondary grief among NICU staff is substantial and under-addressed. StoryTapestry provides a clinician-only reflection space — entirely private from families — where staff can process what they witnessed. Unit leaders can aggregate anonymized reflection themes for staff support without breaching family confidentiality. This dual-purpose architecture follows medical record integration principles we support across clinical memorial infrastructure.
Longitudinal staff contribution. Some staff want to contribute weeks or months after the loss — perhaps after a particularly difficult shift surfaces memory of an earlier case. StoryTapestry keeps staff contribution channels open beyond the acute hospitalization window, with clear staff-facing guidelines about when contribution is appropriate and how to mark the temporal context of later additions. This parallels story accuracy verification practice for decades-later contributions in other memorial contexts.
Advanced Tactics for NICU Staff Story Gathering
Primary nurse designation and continuity. When a family has a primary NICU nurse — the nurse who has cared for the baby across multiple shifts — StoryTapestry can designate that nurse as the family's primary staff contributor, with the family's consent. The primary nurse's contribution thread becomes a continuity anchor across otherwise fragmented shift changes.
Handoff-bridging contributions. NICU nurses already document patient status during shift handoff, and the bridge into medical milestone narrative capture is where clinical observation becomes memorial thread. StoryTapestry provides a light bridge that lets nurses flag a clinical handoff detail as potentially meaningful for the family memorial — with review by the bereavement coordinator before it is offered to the family. This prevents relevant moments from being lost between care and memorial.
Debriefing session integration. Many NICU units conduct bereavement debriefings after losses. StoryTapestry can integrate with debriefing protocols so that — with careful consent practices — thematic learnings from debriefings become available to the care team (never directly to the family unless the family opts in). This approach builds on the bereavement debriefing evidence base documented in NICU fellowship literature.
Trainee contribution pathways. Residents, fellows, and nursing students who rotate through NICU often carry deep learning moments from the families they care for. StoryTapestry provides a trainee-appropriate contribution pathway that acknowledges the developmental context of their observations while preserving family consent as the governing principle. A resident's one-sentence observation may become a tapestry thread that reshapes their career orientation.
Anniversary contribution invitations. On significant anniversaries — a year after discharge, for example — StoryTapestry can, with family consent, invite primary care team members to add new reflections. Some nurses report that a year's distance lets them articulate observations they could not form in the acute phase, which is why careful story accuracy verification matters as time passes between the event and the telling. Anniversary contributions are always skippable and always gated by family review.
Quality improvement feedback loops. Unit leaders can aggregate anonymized staff contribution patterns to identify training needs, emotional load distribution, and workflow opportunities. Nurses who consistently find it difficult to articulate observations may benefit from additional bereavement training; the aggregate data surfaces these needs without exposing individual staff.
For Hospital Bereavement Programs Ready to Capture What Staff Already Witness
Your NICU nurses, respiratory therapists, and care team already witness the moments families wish they could preserve. StoryTapestry builds the infrastructure that turns those observations into tapestry threads families can hold forever. The platform integrates with your unit's existing workflows — shift handoffs, bereavement debriefings, primary nurse designation — and respects every boundary of family consent and clinical privacy. We partner with NICU leadership, bereavement coordinators, and affiliated hospital funeral services to pilot the platform in units where staff contribution will matter most. Contact our hospital partnerships team to schedule a conversation with your NICU leadership and bereavement program. The NICU partnership call runs 60 minutes and covers the staff contribution workflow, the primary nurse designation integration, the bereavement debriefing capture process, and a sample family-facing tapestry with eight staff contributions layered against the family's own narrative.
Pilot engagements include platform access for your NICU bereavement coordinator, two primary nurses, one respiratory therapist lead, and one staff chaplain, plus a named implementation lead who attends the first three bereavement debriefings. Most programs onboard their first family inside four weeks of contract signing and reach protocol-level adoption across all shift teams by month five. Bring your NICU medical director, nurse manager, bereavement coordinator, and one primary nurse representing night shift — the consultation produces a role-mapped implementation plan with a pilot case slate ready to go.