Integrating Medical Milestone Records into Infant Memorial Narratives
The Problem: Medical Milestones Locked Inside Clinical Systems
The CDC Linked Birth and Infant Death Data connects records for roughly 21,000 infant deaths annually in the United States, and each one produces a dense footprint inside electronic health records — vitals logged minute by minute, weight-gain plots, first-bath timestamps, transfusion records, and nursing narratives describing the hand a mother held. Families often do not see any of this during the crisis. After discharge, they receive a discharge summary and a bill. The minute-by-minute record that captured their baby's entire life stays sealed behind chart-access protocols they do not know how to invoke.
Clinical teams feel the gap too. Research in Healthcare IT News on clinical narrative points out that the real story inside a chart is assembled across dozens of note types — nursing flowsheets, respiratory-therapy logs, bedside photos, lactation consults — and that no single view pulls them together. An analysis of document ontology and EHR narratives found that narrative-note volume inside hospital EHRs grows faster than any other chart component, yet families almost never receive a humanized version of it. A review of bereavement support in the NICU emphasizes that grieving parents need individualized narrative records reflecting the specific clinical situation they lived through — not a generic condolence letter.
So the bereaved parent is left with fragments: a bracelet, a footprint card, a memory of a nurse saying "she squeezed my finger." The medical record — often the most complete record in existence — sits inaccessible.
Solution Framework: Weaving Chart Data Into the Tapestry
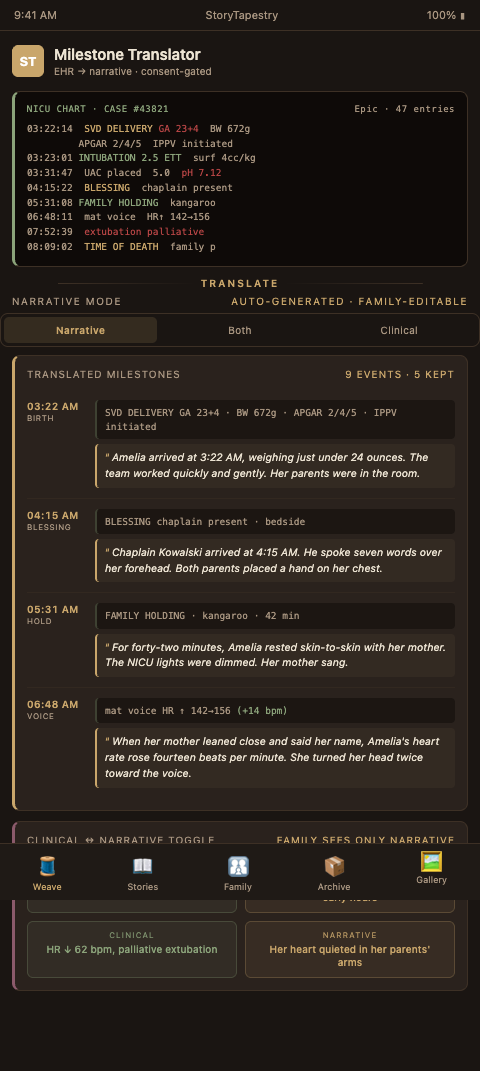
A memorial tapestry works when each fragment carries meaning that parents can feel. Medical milestones are fragments that need translation before they can join the weave. StoryTapestry treats the chart as a thread library: clinicians identify which moments have human weight, translators render them in plain language, and families decide which ones become part of the permanent record.
The extraction step comes first. A structured-narrative model, like the one described in PMC's EHR framework for structured narrative, lets teams pull a small set of marker events out of the chart: admission to the NICU, first skin-to-skin contact, first feed, first open eyes, stabilizing oxygen saturation above 92%, extubation, last weight. These are coded events, not free text, so they can be exported without lifting an entire patient record. StoryTapestry receives them as structured entries and pairs each with a timestamp, a clinician note, and a plain-language caption the bereavement coordinator drafts in collaboration with the family.
The translation step follows. A raw chart entry that reads "PCV 42, Hct stable post-transfusion, resp support PS/CPAP 6/5 FiO2 0.25" means nothing to a parent three weeks later. Translated, it becomes: "By 2:47am, she was breathing more of the room's air than the machine's. Her color came back." The caption preserves the medical truth while honoring the child. The NICU palliative and bereavement framework outlines this dual-register approach — clinical accuracy underneath, family-facing narrative on top — and StoryTapestry implements it as a two-layer record: clinicians see the medical layer, families see the narrative layer, and both are versioned together so neither erases the other.
The weaving step is where the tapestry metaphor becomes concrete. Each milestone becomes a thread. The thread is anchored to a timestamp, which gives it a place in the weave. It connects to the previous and next thread, which creates the visible arc of a life. A stillbirth memorial may have only three or four threads; a 53-day NICU journey may have sixty. Both produce a coherent tapestry because the structure does not require a minimum length. Parents can add photographs, handprints, and voicemails from grandparents around the chart-derived threads, turning a clinical timeline into a life record that still carries clinical authenticity.
Consent is the final pillar. The PMC review on individualized NICU bereavement notes that what one family wants to remember, another wants to forget. StoryTapestry gives families a shelf rather than an inbox: the extracted milestones sit available for review, and the parent chooses which ones to weave in, which ones to keep in a private vault, and which ones to discard. No chart entry auto-publishes.
Bereavement coordinators implementing this framework typically start with a curated list of about twelve milestone types rather than trying to extract everything clinically possible. The list is unit-specific: a Level III NICU working with 24-week micropreemies will include extubation, first oral feed, and kangaroo care; a labor-and-delivery unit handling stillbirth will include last fetal heart tones, delivery time, and the parents' first hold. Starting with a constrained list prevents the tapestry from becoming a chart dump and forces clinicians to think about which moments carry human weight before extraction happens. Teams can expand the list after six months of practice, once the translation rhythm is established and the bereavement coordinator has learned which milestones the families in her cohort actually want woven in.
The two-layer record has a practical implication for bereavement coordinator workflow. Coordinators never write clinical translations alone; they sit with one family member — usually the mother, sometimes the father, sometimes a grandmother who wants the job — and translate each milestone together. The parent hears the clinical reading, says what the moment felt like, and the coordinator drafts the caption on the screen while the parent watches. This collaborative drafting typically runs forty minutes for a three-day NICU stay and produces captions that the family feels they own. When the parent later shows the tapestry to a grandparent, the captions sound like the parent wrote them, because in the sense that matters, she did.
Advanced Tactics for Chart-Integrated Memorials
Three practices separate a meaningful medical-thread integration from a data dump.
First, pair milestones with the clinician who witnessed them. A first-feed entry gains depth when the nurse who fed the baby contributes a two-sentence note. Many NICUs already do this informally in condolence cards; StoryTapestry formalizes it as an optional clinician-caption field tied to each milestone. Teams report that nurses find it a meaningful closure ritual as well.
Second, extract ambient chart data, not only event data. Heartbeat recordings, ultrasound heartbeat tapestry captures, incubator photographs, and SpO2 waveforms can be rendered as ambient textures behind the milestone threads. A six-hour life produces almost no event density, but it produces continuous waveform data that can become visual and auditory background — the hum of the tapestry beneath the threads.
Third, build a retention schedule that respects both sides of the chart. Clinical records are governed by state retention laws and HIPAA, and the narrative-layer record the family keeps has to stand separate from the hospital's clinical record. Draft a handoff agreement with the compliance office specifying that StoryTapestry receives a bereavement-purposed derivative record, not the primary record, with medical privacy consent signed by the personal representative before any extraction. This prevents drift between the hospital's legal record and the family's memorial record.
Narrative-assembly approaches from adjacent fields translate directly. The tools used in dementia memory-care programs — which pull fragments from caregivers, relatives, and medical charts into a single story — map cleanly onto perinatal use because both domains deal with scattered fragments of an under-documented life. Borrow their workflow rather than inventing one.
Finally, run a quarterly audit. Bereavement coordinators review a sample of completed tapestries and check whether the medical threads landed in plain language, whether consent was logged, and whether any clinical jargon leaked into the family-facing layer. This keeps the program from drifting into either over-clinical or over-sanitized territory.
Train a translation guild. Bereavement coordinators doing the translation work alone burn out fast, because each caption requires them to hold clinical knowledge, narrative sensibility, and emotional presence simultaneously. Programs that run well train a small guild of translators — typically a coordinator, a senior L&D nurse, a NICU nurse, and one chaplain — who rotate the translation work and meet monthly to review each other's captions. The guild serves a secondary function: when a nurse who witnessed a milestone is the one translating it, the caption carries the nurse's observation. "She squeezed your finger" is not a chart entry; it is something a nurse heard, remembered, and wrote into the weave.
Build a denial workflow for chart entries the family asks not to include. Some families will read an extracted milestone and say, "I do not want that in the memorial." The system must honor the denial without deleting the underlying chart data, because the chart belongs to the hospital's legal record and cannot be erased by family preference. StoryTapestry supports a "not included" flag on any milestone, which keeps the entry present in the clinical layer of the memorial record but suppresses it in the family-facing tapestry. A family who later changes their mind — at month twelve, at year three, at their adult surviving sibling's request two decades later — can re-surface the denied milestone with one action. Denial is not deletion.
Handle subsequent pregnancies with care. Many bereaved families conceive again, and the subsequent pregnancy's clinical workflow often surfaces reminders of the previous loss. Coordinators should flag bereaved parents at intake of subsequent pregnancies so that the OB team knows which chart events might echo for the family, and so that StoryTapestry can offer the option of adding context to the previous tapestry rather than creating a separate record. A mother at 34 weeks with a rainbow pregnancy who passes the gestational week at which she lost her previous baby may want to add a single thread to the earlier tapestry: "I carried him past you today." Making that possible is part of the infrastructure.
CTA: For Hospital Bereavement Programs Building Chart-Integrated Memorials
Hospital bereavement teams sit on the richest record their families will ever have of their baby's life, and most of it never reaches them. StoryTapestry gives coordinators a structured way to pull medical milestones into a narrative record parents can hold. The 45-minute walkthrough we run with new programs includes your L&D and NICU leads, one representative from your compliance office, and — if possible — your Epic or Cerner analyst, because chart integration is as much an EHR project as it is a bereavement project. We will show the milestone extraction on a sanitized demo case, walk through the two-layer consent flow from admission to year-three memorial access, and demonstrate the compliance handoff model that separates the hospital's clinical record from the family's bereavement-purposed derivative.
Most programs begin with a single unit and a cohort of five families. The first case typically takes three hours of coordinator time from consent through delivered tapestry; by the tenth case, that time drops to forty-five minutes because the translation guild has built a library of milestone-type templates that shorten the drafting work without flattening the captions. We help you stand up the guild, the audit cadence, and the denial workflow in the first quarter. The platform reuses the same narrative assembly tools that dementia memory-care programs rely on, so your coordinators inherit proven fragment-assembly infrastructure rather than early-adopter tooling. Start with a single unit, a single workflow, and a single family at a time.