Building a Life Tapestry from Ultrasound Images and Heartbeat Recordings
The Problem: Prenatal Recordings Are Often the Only Artifacts, and They Sit in Phone Folders
A bereaved father described the USB drive on his nightstand: it held the 12-week ultrasound video, the 20-week anatomy scan, and a 47-second recording of his daughter's heartbeat he had made at the last OB visit by holding his phone up to the doppler speaker. His daughter was stillborn at 32 weeks. The USB drive contained the richest sensory record of her existence — and he had no structure to share it with family, preserve it against drive failure, or layer the context he remembered around each recording.
Research consistently shows that prenatal imaging functions as core memorial material. Legacy-making research in pediatric palliative care documented that tangible legacy items — heartbeat recordings, fingerprint charms, written letters — carry disproportionate significance for bereaved families. Research on continuing bonds with posthumous children traced how prenatal images become objects through which families maintain connection across time. A NICU palliative care study found that 94% of NICU families desired formal memory-making — with imaging artifacts central to that process. Legacy intervention research confirmed digital storytelling legacy work was feasible and accepted by NICU parents. A grounded theory study of 18 bereaved parents documented how memory-making emerges as a core process in neonatal end-of-life care.
Yet most families receive their prenatal recordings as raw files with no surrounding narrative structure. The heartbeat audio sits in a voice memo app. The ultrasound video lives on a CD that no modern laptop can read. The artifact that should anchor a memorial drifts into digital oblivion.
The Solution: Weaving Prenatal Recordings Into the Memorial Tapestry
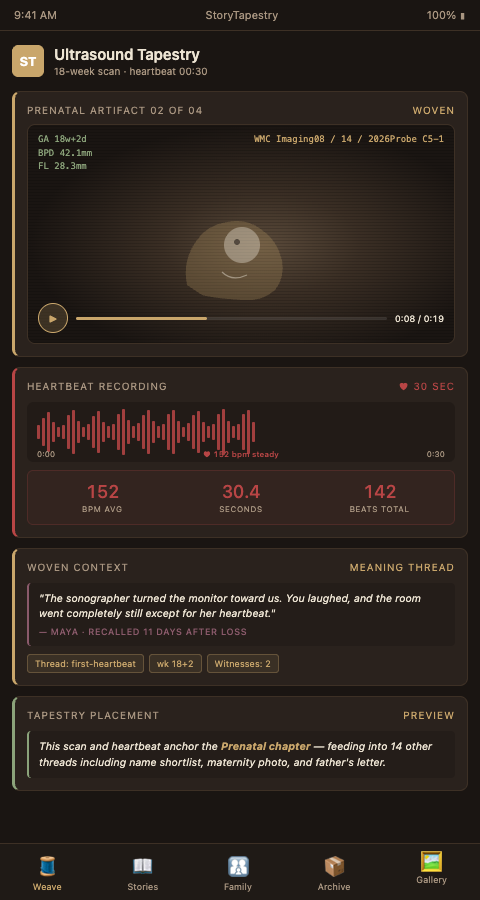
StoryTapestry treats ultrasound images, fetal heartbeat recordings, and related prenatal sensory artifacts as core tapestry threads — as permanent, as contextualized, and as interactive as any other family contribution. The tapestry metaphor works because an isolated ultrasound clip is a single gray-and-black thread; woven with the mother's voice describing the moment, the father's comment, and the nurse's observation, it becomes a visible pattern with meaning.
Multi-format prenatal media ingestion. StoryTapestry accepts ultrasound images, ultrasound video clips, fetal heartbeat audio recordings (whether captured by the sonographer or by family members via doppler), and 3D/4D imaging output. The platform preserves original file fidelity while generating web-viewable versions that families can share without losing archival quality. Northside Hospital's memorial resource guide already recommends ultrasound-based memory-making; StoryTapestry operationalizes this recommendation as structured workflow.
Contextual narrative wrapping. Each uploaded recording sits at the center of a narrative panel with prompts that gather the context the file itself cannot hold: where the recording happened, who was in the room, what the parent was thinking when they heard the heartbeat, what the sonographer said about the baby's position. The raw artifact becomes a thread; the surrounding context becomes the visible weave around it. This approach parallels our broader work on physical artifact digitization for post-loss keepsakes.
Heartbeat waveform visualization. A 30-second heartbeat recording is a waveform as well as audio, and when paired with tangible memorial keepsakes becomes one of the most durable threads a family can hold. StoryTapestry generates a permanent visual representation of the heartbeat rhythm that families can export as printed art — a silent memorial that works in spaces where audio playback is not appropriate. Hospital-affiliated funeral homes increasingly offer heartbeat waveform keepsake prints; StoryTapestry automates the file preparation and preservation layer.
Ultrasound annotation layer. Families can draw or annotate directly on their stored ultrasound images — circling the hand they fell in love with, marking the profile they remember best, adding a short text note beside a specific feature. These annotations persist as their own layer, preserving the image unaltered while adding the family's voice to the visual record.
Consent-based multi-viewer access. Prenatal media is intimate. StoryTapestry uses granular consent controls: parents decide which specific recordings are visible to the extended family, which are visible only to the grandparents, and which remain entirely private. A 4D ultrasound video may sit at the core of the memorial but only appear to viewers the parents have explicitly approved. Tangible memory keepsakes follow the same consent-controlled distribution logic.
Advanced Tactics for Prenatal Media Memorial Integration
Chronological ultrasound timeline assembly. When a family has multiple ultrasounds from across pregnancy — 8 weeks, 12 weeks, 20 weeks, 32 weeks — StoryTapestry assembles them into a chronological timeline with gestational age, annotations, and narrative context at each point. The timeline becomes a visible growth record, and parents report that this structure helps them hold the reality of the pregnancy their baby experienced even if life outside the womb was brief. This mirrors the interactive record timelines approach we use in other memorial contexts.
Sonographer contribution channel. Sonographers often develop a relationship with a pregnant family across repeated visits. StoryTapestry provides a consent-controlled channel where sonographers — with family invitation — can add their own observations about moments the parents may not have fully taken in during the scan. A sonographer's note that "she kicked every time her mother laughed" becomes a permanent tapestry thread.
Heartbeat-to-song pairing. Some families want their baby's heartbeat paired with a specific song — a lullaby, a hymn, a song the parents played during pregnancy. StoryTapestry provides audio pairing tools that preserve both the heartbeat and the paired song as linked threads, with clear attribution and (where needed) rights-respectful handling of copyrighted music, the same sequencing logic that powers our interactive record timeline work in other bereavement niches.
Post-discharge additional capture. Not all prenatal media is captured during the hospital stay. Parents sometimes have old ultrasound recordings on outdated devices, or they recall audio recordings buried in their phone's voice memos from months earlier. StoryTapestry includes a post-discharge upload workflow that lets families add newly surfaced recordings weeks or months later without having to re-enter the original narrative.
Integration with 3D printing and shadow box fulfillment. Affiliated funeral homes increasingly offer 3D-printed heartbeat waveform pendants, shadow boxes with printed ultrasound overlays, and similar tangible keepsakes. StoryTapestry exports media and annotation data in formats that 3D printers and print shops can fulfill directly — reducing the re-entry burden on grieving families and creating a seamless bridge between the digital tapestry and the physical keepsake.
Archival redundancy and long-term preservation. USB drives fail. Phones die. StoryTapestry's archival layer preserves original media in multiple geographic data centers, with family-controlled export options, extending the same physical artifact digitization rigor we apply to post-loss keepsakes. The memorial persists through hardware generations the original recording medium will not survive.
For Hospital Bereavement Programs Ready to Preserve Prenatal Artifacts
Prenatal ultrasound images and heartbeat recordings carry disproportionate weight for bereaved families. If your hospital's bereavement workflow hands families a CD or a ZIP file at discharge, the system is losing memorials every year to hardware failure, app migration, and digital neglect. StoryTapestry preserves these artifacts inside a structured tapestry your bereavement coordinators can hand to families as a lifetime resource rather than a temporary file. We work with perinatal teams, affiliated funeral services, and sonography departments to integrate sensitively with existing consent and disclosure practices. Contact our hospital bereavement partnerships team to discuss a pilot that includes your sonography department and affiliated funeral home partners.
The partnership consultation runs 60 minutes and covers DICOM ingest from your sonography PACS, fetal heart monitor audio capture from your L&D triage suite, the sonographer contribution channel, and the archival redundancy stack that preserves every artifact across three geographic data centers. Pilot engagements include platform access for your bereavement coordinator, two sonographers, and one PACS administrator, plus a named clinical implementation lead who handles the integration with your existing imaging workflow. Most programs complete sonography integration within six weeks and onboard their first family the week integration closes. Bring your bereavement coordinator, your lead sonographer, one PACS administrator, and a representative from your affiliated funeral home's keepsake fulfillment workflow — the consultation produces a four-role implementation plan with a clear integration timeline.