Scaling Perinatal Memorial Programs Across Hospital Networks
The Fragmented State of Network-Wide Perinatal Memorial Care
A regional health system with 14 labor and delivery units reviewed its bereavement documentation after a parent complaint. Two sites had no written protocol. Seven had protocols from different decades. The flagship hospital had a dedicated coordinator. The community hospitals had a charge nurse improvising. The result was that a mother who delivered a stillborn at 34 weeks might receive hand and foot molds, photographs by a trained volunteer, and a keepsake book at one site, while 40 miles away a different mother received only a printed sympathy card tucked into her discharge paperwork.
The implementation inconsistency documented across settings is not a secret within hospital administration. It produces measurable outcomes: parents at under-resourced sites score higher on prolonged grief measures, sibling inclusion drops, and clinician turnover rises as nurses burn out from emotional labor without structure. A systematic review of perinatal palliative care pathways confirmed that the absence of structured rollout produces uneven care across otherwise similar hospitals.
Network-wide scaling fails for three reasons. First, each site has a unique bereavement champion whose expertise lives in their head rather than in documented workflow. Second, enterprise EMR configurations rarely include memorial program fields, so documentation falls outside the system of record. Third, leadership often views perinatal memorialization as a local cultural issue rather than an infrastructure problem with an operational answer.
The Tapestry Framework for Multi-Hospital Memorial Rollout
StoryTapestry treats a hospital network the way a master weaver treats a commissioned series: each tapestry carries its site's distinct texture and color palette, but every panel is woven on compatible looms with threads that meet the same tensile standard. The metaphor matters because scaling perinatal memorialization does not mean erasing local practice. It means giving every site threads, tools, and frames that interoperate while the loom keeper at each location still chooses the pattern.
Begin with loom standardization. Every participating hospital receives the same intake form that captures the four essential thread types: Medical Team Moment Documentation entered by L&D, NICU, and chaplaincy staff; Micro-Moment Amplification for parents who want to preserve a single touch or breath; Trauma-Informed Guided Storytelling prompts that adapt to gestational age and circumstance; and Sibling and Family Inclusion Pathways that capture how a 4-year-old said goodbye. These are the warp threads that feed every downstream hospital funeral coordination task, and they run through every site's tapestry to hold the structure.
Then localize the weft. The flagship academic center may have a dedicated bereavement coordinator who conducts structured interviews at 24 and 72 hours. A community hospital may have one trained RN on each shift. Both sites produce compatible tapestries because the platform adapts to staffing rather than demanding identical workflows. Resolve Through Sharing, which has trained over 65,000 professionals globally since 1981, demonstrates that a shared training foundation accommodates local staffing realities without losing care quality.
Sequence the rollout in three phases. Phase one is flagship deployment: the site with existing bereavement infrastructure adopts the digital tapestry platform and documents its workflow. Phase two is paired rollout: each community site pairs with the flagship for 12 weeks of shadowed implementation. Phase three is autonomous operation with quarterly network convenings. The perinatal bereavement policy standardization documented across a 16-hospital system confirmed that structured three-phase planning produced more durable adoption than simultaneous network-wide launch.
Build cross-site governance that honors clinical judgment. A network bereavement council with representatives from every site meets quarterly. They review tapestry completion rates, parent feedback, and clinician feedback. They do not mandate uniformity. They surface patterns. When a community site discovers that their Spanish-speaking families preferred voice notes over written entries, that insight becomes an option available to every other site rather than a requirement imposed on them. This is how StoryTapestry scales without flattening.
Integration with hospital funeral coordination becomes standardized at the network level. Each site's referral pathway uses the same data handoff format, so a parent who delivers in one community hospital but chooses a funeral home near their flagship specialist receives a seamless transition. Similarly, memorial program funding aggregates at the network level, which unlocks grant scale unavailable to single-site programs. Organizations that have solved analogous multi-site challenges, including bereavement program scaling in memory care networks, offer transferable rollout patterns.
The phased rollout sequence matters more than most networks assume. Networks that attempt simultaneous launch across fourteen or sixteen sites almost always watch four to six sites stall within the first year because the launch overwhelmed local champions who did not have time to learn the platform while continuing clinical work. Phased rollout, by contrast, lets the flagship site develop internal expertise that becomes the training resource for the community sites. By the time the paired rollout phase begins, the flagship's bereavement coordinator has resolved the first wave of workflow questions and can mentor community peers through the same questions in half the time. Networks that document this mentorship explicitly — scheduling named shadow shifts, paying for travel between sites, and treating flagship coordinators as network-wide faculty rather than just local practitioners — produce faster, stickier adoption than networks that leave mentorship informal.
Local clinician authorship is the under-documented variable. In every network that rolls out a standardized program successfully, the platform's default workflows are presented at each site as a starting point that the local clinical team is invited to modify within the network standard. A community hospital whose Spanish-speaking families prefer voice notes over written prompts must be able to modify the default intake to prioritize voice capture without breaking compatibility with the network's aggregate reporting. StoryTapestry supports this through a configuration layer that exposes modifiable defaults — prompt ordering, modality priority, anniversary touchpoint calendar — while keeping the underlying data schema constant. Local clinicians experience the platform as theirs. Network administrators still receive comparable data. Both needs are satisfied because the architecture separates configuration from schema.
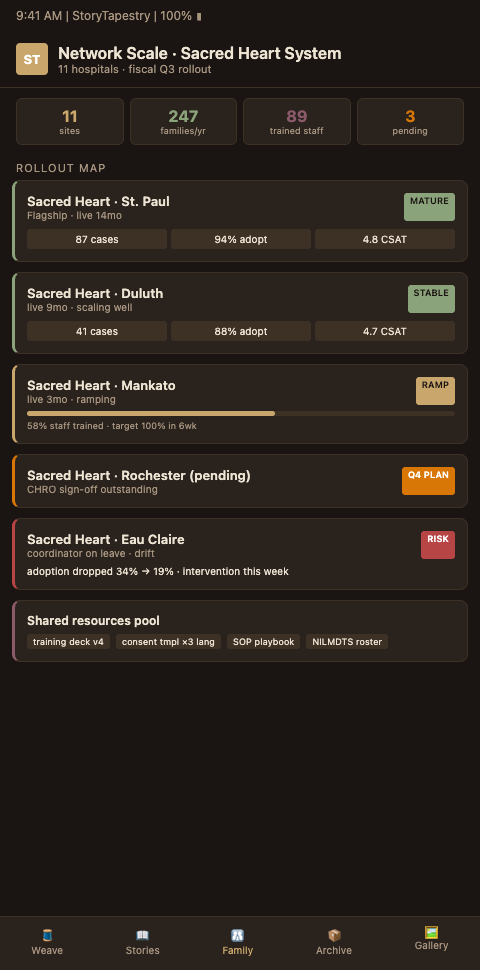
Advanced Tactics for Multi-Site Memorial Program Consolidation
Rollout maturity requires attention beyond the initial three phases. Four tactics distinguish networks that sustain the program from those that watch it decay within 18 months.
Establish a network-level bereavement data standard before technology selection, alongside a plan for memorial program funding that can absorb the standard once proven. The AWHONN Certificate Program for Perinatal Bereavement Care provides a vocabulary for intake fields, certification milestones, and documentation categories. Adopt that vocabulary as your network standard. When every site uses identical field names for loss type, gestational age, parent preferences, and memory-making activities completed, data aggregation and benchmarking become tractable rather than an annual consulting project.
Build floating bereavement specialists who rotate across sites. A network of 10 hospitals cannot afford 10 full-time bereavement coordinators. It can afford three floating specialists who rotate on a 90-day cycle, each spending 30 days at each of three sites, then rotating. This model distributes deep expertise, creates cross-site pollination, and provides coverage during bereavement coordinator vacation or parental leave. The collaboration across L&D, NICU, and pastoral care documented as essential becomes easier when specialists themselves cross sites.
Embed memorial documentation into existing EMR workflow rather than building a parallel system. Nurses will not chart twice. When StoryTapestry entries flow from Epic or Cerner smart phrases, charge nurses can capture Medical Team Moment Documentation within their routine charting. This integration requires upfront IT investment but produces near-universal clinician adoption rather than the 30-40% adoption typical of parallel documentation platforms.
Measure network outcomes, not just site outcomes. Parent grief measures at 12 months should be aggregated at network level with site-level comparisons, borrowing lessons from bereavement program scaling work in other domains. When one site's scores lag, the network council investigates rather than the site defending itself. This culture shift takes two to three years but transforms memorial care from a local virtue to a shared responsibility.
Build a network-wide mortality and morbidity review process that includes bereavement coordinators. Most hospital M&M conferences run unit-by-unit and treat bereavement follow-through as an afterthought to the clinical review. Networks that mature their memorial program bring bereavement coordinators into M&M review with structured contributions: what the family needed at discharge, what was missed, what the tapestry captured that the chart did not. A community hospital coordinator who presents quarterly findings to the flagship's M&M committee becomes a peer to the maternal-fetal medicine specialists rather than an administrative function, and the visibility raises both clinical standards and program morale. Within eighteen months, the coordinators themselves become the network's most effective internal advocates.
Standardize the data de-identification pipeline before sharing across sites. Even within a single health system, cross-site data sharing must satisfy institutional review boards and HIPAA requirements at every participating site. Networks that build their de-identification pipeline in year one can aggregate outcomes data legally by year two; networks that defer the compliance work find themselves with interesting cross-site patterns they cannot act on because the legal framework is missing. StoryTapestry's network edition includes a de-identification layer that removes direct identifiers and bins rare loss types into broader categories to prevent re-identification, but the hospital system's compliance office still reviews and approves the layer before aggregation begins. Investing in this infrastructure early pays back repeatedly when grant applications, quality improvement projects, and academic publications all need the same clean data source.
Design the network for leadership turnover rather than leadership stability. The executives who sponsor a multi-site memorial program at launch are often not the same executives who must defend its budget at year three. Networks that build documentation, outcomes evidence, and community advocacy into the program's first year survive these transitions; networks that rely on executive patronage watch the program lose priority when a new CEO rotates through. Quarterly briefings to the board's quality committee, annual external-review presentations at regional perinatal conferences, and named community philanthropy tied to the program all create the political durability that outlasts any single leader.
Weave One Coherent Tapestry Across Your Network
Hospital bereavement programs operating across multiple sites face a choice: watch each hospital reinvent perinatal memorial care in isolation, or build a shared infrastructure that honors local clinical judgment while delivering consistent family experience. StoryTapestry provides the loom, threads, and frames to weave one coherent tapestry across every site in your network. Our implementation team has rolled out programs across networks ranging from three-site community systems to 22-hospital academic networks.
The network readiness assessment is a structured two-week discovery engagement with your system's chief nursing officer, maternal-child health director, and a representative bereavement coordinator from both flagship and community sites. The assessment maps your current state across four dimensions: intake and documentation consistency, staffing depth for bereavement roles, handoff quality to affiliated funeral homes, and outcome measurement maturity. The output is a phased rollout plan that identifies which sites are ready for flagship deployment, which need paired implementation support, and which require foundational work on intake workflows before the platform rolls out.
Request a network readiness assessment to map your current state and design the phased rollout that fits your operational reality. We can typically complete the assessment within four to six weeks and present findings to your system's quality and safety committee at their next quarterly meeting. The goal is not to arrive with a predetermined rollout timeline but to understand your system's operational reality, clinical culture, and patient population well enough to recommend a sequence and pace that your staff can actually sustain over the three to five years the rollout will take.