Training Labor and Delivery Staff in Compassionate Story Gathering
The Training Void in Labor and Delivery Perinatal Loss Care
An L&D nurse with 14 years of experience described her first stillbirth encounter: a 38-week delivery with no advance warning. The charge nurse told her to "just be present." She did not know whether to make eye contact with the mother or look away. She did not know whether to name the baby or call him "the baby." She did not know whether to offer hand molds or photographs. She produced what she could from instinct. Seventeen years later, she still does not know whether her care helped or harmed that family.
The 2024 communication training research documenting that 38% of U.S. hospitals report no L&D perinatal loss training quantifies the void. A scoping review of nurse and midwife perinatal bereavement preparation confirms that preparation varies wildly across institutions, with many nurses entering bereavement care scenarios after only brief informal orientation. The American Nurse publication on perinatal bereavement notes that training must span L&D, NICU, mother-baby, and pastoral care rather than resting in a single specialty.
The consequence for families is inconsistent care. The consequence for clinicians is secondary traumatic stress, moral injury, and eventual departure from L&D practice. Neither consequence is inevitable. Training works when it is designed as a clinical skill rather than a wellness offering.
The StoryTapestry Framework for Training L&D Staff in Compassionate Story Gathering
StoryTapestry approaches L&D training the way a master weaver trains apprentices: through graduated practice on safe looms, with explicit attention to both the technical skills of weaving and the emotional posture that allows the weaver to hold difficult threads without breaking them. The training framework blends didactic content, simulation practice, and platform integration so that skills acquired in training transfer directly into clinical workflow.
Module one establishes the clinical posture. Compassionate story gathering begins with nurse self-regulation. A nurse whose own nervous system is dysregulated cannot create conditions for parents to access their own experience. The module covers grounding techniques, pacing principles, and the specific posture shifts that signal availability without intrusion. The perinatal bereavement training RCT research on confidence impacts confirms that training increases clinician confidence measurably, which translates to better family experience.
Module two teaches the story gathering protocol. Nurses practice opening invitations: what would you like me to know about your baby? They practice sustained attention without rushing. They practice documentation that captures the parent's own language rather than clinical paraphrase. The tapestry metaphor enters here. Each parent utterance is a thread. The nurse's job is not to interpret the thread but to preserve it accurately so it can be woven into the broader tapestry the family will carry forward.
Module three covers the four tapestry thread types that L&D staff contribute directly. Medical Team Moment Documentation captures clinically significant observations parents may not witness: the baby's response to touch during delivery, breathing patterns, moments of eye contact. Micro-Moment Amplification captures parent-observed moments that staff can validate and preserve. Trauma-Informed Guided Storytelling training teaches nurses to offer graduated prompts that meet parents where they are rather than demanding articulation parents cannot access. Sibling and Family Inclusion Pathways training teaches nurses to invite family members present in the room into the tapestry as contributors rather than spectators.
Module four addresses documentation inside the platform. Nurses practice adding threads during a simulated delivery scenario. They learn to tag entries by moment type, timestamp, and consent level. They learn to hand off the tapestry to next-shift staff through structured notes, using the same OB unit coordination infrastructure that coordinators use for post-discharge care. The platform's built-in trauma-informed prompts guide nurses through moments when they feel paralyzed. This integration is why the training experiences of OB nurses documenting positive changes in bereaved care translate into durable practice rather than transient conference enthusiasm.
Module five is simulation-based practice with debriefing. Nurses participate in 45-minute scenarios with trained standardized parents who present varying loss circumstances. After each scenario, a trained facilitator debriefs with specific attention to posture, language choices, and documentation completeness. Programs adopting the AWHONN Certificate Program interprofessional certification can align StoryTapestry training with certification competencies, producing recognized credentials alongside platform fluency.
Training quality benefits from cross-functional coordination with OB unit coordination infrastructure so that trained nurses hand off to trained coordinators without gap. Hospital network scaling approaches allow training curricula to propagate across sites without loss of fidelity. Programs adopting sensitive interview training approaches in memory care contexts can transfer many curriculum elements to perinatal training with appropriate adaptation.
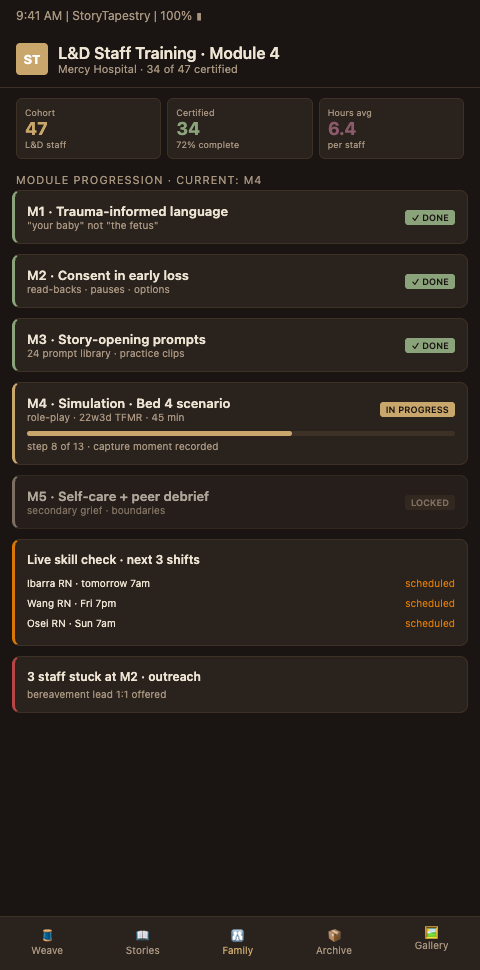
Advanced Tactics for Sustaining L&D Bereavement Training Over Time
Programs that launch training and then watch skills erode within 18 months miss the reinforcement tactics that produce lasting change. Four advanced tactics distinguish programs that sustain competence from programs that re-train annually without improvement.
First, build monthly case review rounds. Every L&D unit that implements bereavement training should host monthly case reviews where a recent case is presented anonymously with specific attention to story gathering choices, documentation quality, and family outcome. The AWHONN certificate program framework supports ongoing case review as part of certification maintenance. Case reviews convert individual learning into team learning and surface practice drift before it becomes entrenched.
Second, pair new graduates with experienced bereavement-trained preceptors for their first three loss encounters, leaning on hospital network scaling infrastructure so that preceptors can rotate across sites when the home unit lacks one. The preceptor does not take over the encounter. She observes, supports, and debriefs. This apprenticeship model produces graduates who enter autonomous practice with supervised experience rather than solo anxiety. It also distributes emotional labor so no single nurse carries the full weight of teaching new graduates through traumatic encounters.
Third, build a peer support protocol for nurses after difficult cases. The research on perinatal bereavement training confirms that clinician wellness predicts sustained practice quality. After every stillbirth or neonatal death, nurses who provided care receive a structured peer check-in within 72 hours. This is not mandatory therapy. It is a brief conversation with a trained colleague that validates the emotional labor and identifies nurses who may benefit from deeper support.
Fourth, measure training outcomes across the family experience chain, drawing on sensitive interview training evaluation rubrics already validated in memory care contexts. Pre and post training competence scores are necessary but insufficient. Programs should also measure family experience scores 6 weeks post-loss for cases handled by trained versus untrained nurses, clinician retention rates, and nurse-reported confidence at 6 and 12 months post-training. Triangulated measurement protects training budgets during leadership transitions.
Invest in Training That Transforms Compassionate Care Into Clinical Competence
Hospital programs that want their L&D staff to handle perinatal loss with the same clinical confidence they bring to routine deliveries can adopt StoryTapestry's integrated training curriculum. The curriculum aligns with AWHONN certification, builds directly into platform workflow, and provides the simulation infrastructure and ongoing reinforcement tactics that sustain competence. Our training team works with hospital education departments to design cohort schedules, secure CEU accreditation, and build the internal preceptor network that carries skills forward after initial training ends. Request a training consultation to map what comprehensive L&D bereavement training looks like in your specific staffing environment. The consultation runs 60 minutes and covers the four-module curriculum map, the simulation infrastructure requirements, the preceptor certification pathway, and the family experience measurement protocol that tracks training impact at the 6-week post-loss mark.
Cohort enrollments include training access for up to 18 L&D nurses per cohort, simulation lab time structured across four sessions, CEU accreditation handling through your hospital education department, and a named training lead who shadows the first three post-training case debriefings. Most programs complete the first cohort within 12 weeks of contract signing and see measurable family-experience score improvements by month six. Bring your L&D nurse manager, education department director, bereavement coordinator, and one charge nurse representing night shift — the consultation produces a staffing-environment-specific training plan the four of them can present to hospital leadership and their union partners before cohort enrollment opens.