Connecting VA Bereavement Services with Funeral Home Story Collection
The Problem: VA Bereavement and Funeral Story Work Run on Separate Tracks
A funeral director serves a Gold Star family whose husband died by suicide six months after leaving the Army. The family qualifies for VA Bereavement Counseling and Vet Center services, but no one at the funeral home mentions the resource, and the family learns about it nine months later from a friend. Meanwhile, the funeral home's memorial website shows a static obituary page that captured none of the unit stories or deployment details the VA Bereavement Counselor would later help the family access as part of grief processing.
The numbers expose the scale of this miss. More than 500,000 veterans die every year, most outside VA facilities and almost all through private funeral homes (NHPCO). The VA operates 206 community-based Vet Centers offering free bereavement counseling and has built a dedicated REACH guide connecting veterans and families to grief resources (Vet Centers; VA REACH; VA). TAPS runs a 24/7 helpline and peer support network specifically for military loss survivors, and the Veterans Crisis Line reaches survivors at 988 + 1 for active crisis (TAPS; Veterans Crisis Line).
We Honor Veterans, coordinated with NHPCO, has enlisted more than 3,000 hospices in compassionate-listening practices for veterans at end of life (We Honor Veterans; NHPCO). The hospice and VA bereavement systems are wired for story collection and grief support. Funeral homes, the connective tissue between end of life and memorial, rarely bridge these systems into their memorial workflow.
Solution Framework: Weaving VA Bereavement Into the Memorial Tapestry
Connecting VA bereavement services to funeral home story collection works when the memorial tapestry becomes the shared artifact across both systems. StoryTapestry gives funeral homes an architecture that references, links, and integrates VA and adjacent bereavement resources so every family receives the full support network alongside the memorial, and every memorial carries the story depth that bereavement processing benefits from.
The integration operates on four threads. First, the resource-surfacing thread: at intake, the platform generates a family-facing resource packet covering VA Bereavement Counseling eligibility, the local Vet Center contact, TAPS 24/7 helpline, the Veterans Crisis Line, and the VA REACH grief guide (VA; TAPS; Veterans Crisis Line; VA REACH). Families receive the full support map before they leave the funeral home.
Second, the upstream-story-handoff thread: when a veteran received hospice care at a We Honor Veterans partner, the funeral home can coordinate transfer of the stories the hospice team gathered through compassionate-listening practice (We Honor Veterans). StoryTapestry accepts hospice contributions as tapestry threads with clear attribution, so the memorial extends upstream of death rather than beginning at the funeral intake. This workflow parallels funeral home community gaps where similar upstream handoffs consolidate fragmented story sources.
Third, the bereavement-counseling-integration thread: Vet Center bereavement counselors work with families who often benefit from reviewing memorial content as part of grief processing. The tapestry provides shareable, counselor-accessible views so the family's therapist can engage with the memorial if the family chooses. This is not a clinical integration but a family-consent integration: the tapestry becomes material the family may bring into counseling sessions.
Fourth, the comrade-survivor-support thread: former unit members contributing to the memorial are themselves often bereaved by the loss, and many fall outside traditional family bereavement frameworks. The platform surfaces comrade-specific support pathways through TAPS peer support, the Vet Center community services, and VSO chaplaincy so contributing comrades receive the resources they may be quietly needing (TAPS; Vet Centers).
Unit Comrade Outreach Network coordinates comrade contribution and comrade bereavement support inside a single workflow. Deployment Timeline Reconstruction provides the structure around which VA-referred narrative depth accumulates. Classified-Aware Story Frameworks protect contributions that might otherwise be withheld from counselors or family. Dual-Life Narrative Integration binds the VA systems connected to the service life with the civilian systems connected to post-service years.
This integration pattern echoes the way funeral home military service connects to federal memorial infrastructure, and it depends on the same military terminology directors fluency that lets funeral staff navigate VA terminology alongside the family.
The Vet Center model deserves particular attention because its cultural approach aligns with the warrior ethos in ways clinical mental health settings often cannot match. Vet Centers staff themselves with veterans to the greatest extent possible, operate outside the VA medical system so veterans do not need to navigate enrollment procedures to access bereavement support, and offer services in community storefront settings rather than hospital environments. A funeral home that actively refers families to their local Vet Center creates a pathway that bereaved military survivors genuinely use, and the resulting grief trajectory often produces clearer, more stable family relationships around the memorial tapestry over time.
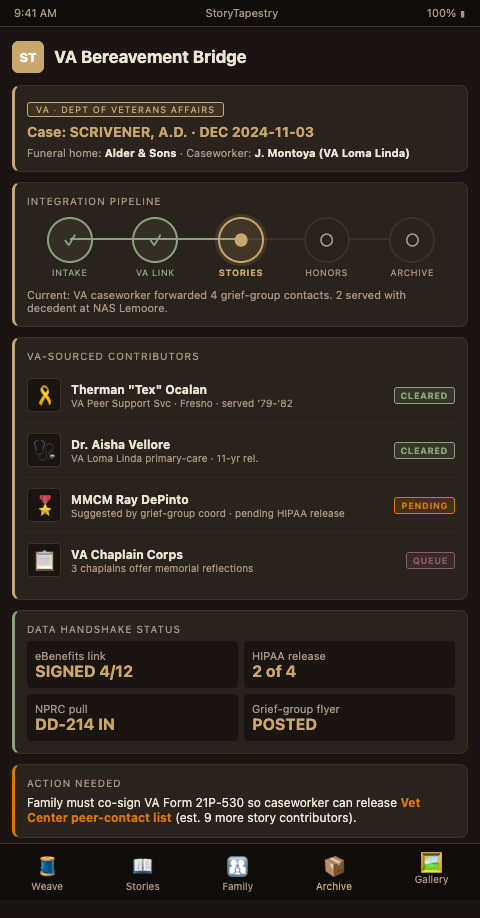
Advanced Tactics for VA Integration in Funeral Practice
Build the resource packet into your standard veteran intake. A printed and emailed packet covering VA Bereavement Counseling eligibility, the local Vet Center address and phone, TAPS helpline, Veterans Crisis Line, and the VA REACH grief guide takes five minutes to generate and removes the number-one regret families report: not learning about free VA grief resources until months after the funeral (VA; TAPS).
Identify your local Vet Center and introduce the funeral home. The 206 Vet Centers operate at community scale, and the bereavement counselor serving your region usually welcomes direct contact from funeral professionals. A 15-minute phone introduction establishes referral pathways both directions: you refer families to them, and they refer families to you when grief processing surfaces memorial needs (Vet Centers).
Coordinate upstream with hospice when the veteran received end-of-life care through a We Honor Veterans partner. Ask the hospice social worker whether the team gathered stories during care, and whether those can be transferred with family consent for memorial use. Hospice story archives often hold the most recent narrative material the veteran produced and significantly enrich the tapestry (We Honor Veterans).
Reference TAPS specifically for military loss survivors. The 24/7 helpline connects survivors to trained peers, and the annual TAPS National Military Survivor Seminar is transformative for many bereaved families (TAPS). Funeral directors who mention TAPS by name rather than listing "national grief resources" earn trust in military families who recognize TAPS as culturally trusted.
Treat the Veterans Crisis Line as a safety reference, not a general resource. The 988 + 1 line reaches trained counselors for veterans and their families in active crisis, and including it in the resource packet is appropriate; invoking it during crisis moments is essential (Veterans Crisis Line). Train every staff member who interacts with families on the number and what it covers.
Follow up at the 30-day, 90-day, and one-year marks. VA Bereavement Counseling eligibility runs on timelines that many families do not initially engage with. A soft outreach at each mark, referencing the tapestry and the VA resources, repositions support for families whose grief landed on a different schedule than the funeral.
Build relationships with the veterans service officers in your community. Accredited VSOs through the American Legion, VFW, DAV, and county veterans service office programs help families navigate VA survivor benefits, including Dependency and Indemnity Compensation (DIC) and burial benefits. A funeral home that can refer the widow to a specific accredited VSO who responds quickly and handles the paperwork competently earns trust that compounds across the bereavement process. StoryTapestry's resource packet can include the specific VSO names and contact information rather than generic organizational references, which raises the conversion rate on referrals dramatically.
Track which families engage with which referrals and share outcome data across your staff. If your last twelve veteran families all ignored the TAPS referral but all followed through on the Vet Center referral, that pattern tells you something about your community's cultural fit with each resource and helps you prioritize which referrals to emphasize in conversation. Treat the resource packet as a living document that improves based on family feedback rather than a static handout. Families appreciate when the funeral home's recommendations reflect the actual experiences of other military families in the community.
Attend an annual VA-hosted training or conference when available. VA regional offices periodically host funeral director training on military honors, burial benefits, and survivor support pathways. Sending at least one staff member annually builds institutional relationships and keeps your firm current on policy changes that affect veteran family support. The costs are modest and the referral relationships built at these events often generate intake volume far exceeding the training investment.
Bridge VA Bereavement Into Your Memorial Workflow
Veteran Memorial Programs that connect VA bereavement resources to memorial tapestries serve families on both grief and legacy dimensions simultaneously. StoryTapestry packages the VA Vet Center, TAPS, Veterans Crisis Line, and We Honor Veterans references into your memorial intake workflow without requiring new staff training or partnership negotiation. Reach our Veteran Memorial Programs team to activate the VA integration for your next veteran family, and stop the nine-month gap between funeral and bereavement support that families should never have to navigate alone.
The activation walkthrough covers specific Vet Center identification for your region, introduction templates your firm can use to open direct relationships with local bereavement counselors, and the hospice handoff workflow for the We Honor Veterans partner hospices in your service area. Firms in regions with high veteran density, such as the communities around Fort Bragg in North Carolina, the Hampton Roads Navy and Marine population, San Diego's Navy and Marine concentration, the Texas triangle of Fort Hood, Fort Bliss, and San Antonio medical/military installations, and the Pacific Northwest clusters around Joint Base Lewis-McChord and Whidbey Island, typically see the deepest value from the full integration because their caseload touches VA resources with high frequency.
Firms serving smaller veteran populations benefit equally from the workflow structure because the few VA engagements they handle each year need to be handled with the same fluency as the higher-volume firms. The Veteran Memorial Programs team configures the platform for your specific community and walks your intake staff through the referral conversations that convert federal-resource awareness into actual family support during the months after the funeral.